Authors: Edward H. Suh, MD†; Liliya Abrukin, MD, MPH†; David Bodnar, MD‡; Gerardo Chiricolo, MD§; Nicholas Gavin, MD, MBA, MS†; Johnathon LeBaron, DO||; Laura Melville, MD, MS§; Marie-Laure Romney, MD, MBA†; Manish Sharma, DO, MBA||; Amos J. Shemesh, MD‡; Peter A.D. Steel, MA, MBBS‡; Brenna M. Farmer, MD, MBA, MS‡
New York Presbyterian COVID-19 Evaluation Pathway
- This evaluation pathway was developed via an iterative process, with input from leadership/academic representatives across the campuses that compose the New York Presbyterian Hospital system.
- The pathways outlined in this guideline reflect the best evidence available at the time, based on literature from China, Europe and the United States.
- The group was able to incorporate real-time feedback from the different institutions; this was critically important as several institutions experienced the surge earlier than others. This protocol reflects the clear need to create a safe outpatient follow-up pathway for patients who would ordinarily be treated as inpatients. Adjustment may be necessary based on the resources available at each facility and to the patient.
- Access to outpatient pulse oximeters, oxygen concentrators and close telehealth follow up are crucial to the ability to discharge this moderate risk cohort.
- In addition, moderate risk patients must have the following in place if they are to be discharged:
- Assistance at home, to limit exertion and facilitate calling 911 if any worsening of clinical status
- A working phone number, in order to participate in the follow up program
- Understanding of how to use the provided devices: pulse oximeter +/- O2 concentrator
- A period of observation in the ED to ensure stability
- These guidelines do not replace clinical judgment, but rather serve to inform clinicians across a broad spectrum of training so as to risk stratify patients with this illness for which there is so little evidence base to draw from.
COVID-19 Evaluation may Include:
COVID-19 Screening Laboratory Panels differ by site but may include:
- Complete Blood Count with differential
- Lymphopenia may be present*
- Thrombocytopenia may be present*
- Complete Metabolic Panel
- Renal insufficiency may be present*
- Transaminitis may be present*
- SARS-COV2 PCR test
- Procalcitonin
- Blood cultures
- Urinalysis
- Urine Culture
- Venous Blood Gas
- Lactate Dehydrogenase*
- Creatine Kinase*
- Troponin or High-sensitivity troponin*
- Ferritin*
- C-Reactive Protein*
- PT/INR
- PTT
- D-dimer*
*abnormal finding may be used for risk stratification
COVID-19 Screening Imaging Studies:
In general, imaging is not required for screen, particularly in low risk patients.
- Chest Radiograph
- Portable is preferred for infection control purposes
- Chest Computed Tomography
- Not a preferred method for diagnosis due to infection control measures required between patients
Evaluation Pathway
(See Figure 9.1 below)
Low Risk:
Clinically mild illness with normal vital signs, age <50, O2 saturation >94% and respiratory rate <22
- Obtain an exertional O2 saturation. If greater than 90% after 1 minute of walking in place at the bedside:
- No routine chest x-ray, unless other indication
- No viral testing if meeting all the above
- If the patient has exertional O2 desaturations below 90%, moderate risk evaluation should occur
Moderate Risk:
O2 saturation 90-94%, respiratory rate ≥22 OR Age ≥50 and co-morbidities:
- hypertension
- COPD
- diabetes
- obesity
- cardiovascular disease
- lung disease
- cancer
- immunosuppression
- renal disease
Obtain labs and imaging as clinically indicated, including laboratory studies to aid in risk stratification: LDH, CRP, ferritin, d-dimer, others based on infectious disease and hospital epidemiology input.
Chest radiograph commonly shows bilateral opacities.
Many of these patients will be admitted.
After a period of observation and if no indication for admission consider the following before discharge:
- Patient must have a working telephone.
- Patient must have assistance at home to limit exertion.
- Patient must be able to participate in a follow-up program.
- Telehealth visits may be very useful for monitoring these patients, if available.
- Consider sending patient home with a pulse oximeter and or supplemental oxygen.
- If that is not possible these patients should be admitted
- If exertional O2 saturation is between 90-92%, discharge home with supplemental O2
High Risk:
Critically ill, respiratory distress, significant tachypnea/work of breathing or hypoxia, shock, or evidence of clinical deterioration while in the ED
- Obtain labs and imaging
- Consult critical care
- Utilize supplemental oxygen: non-rebreather, nasal cannula, or both together
- If negative pressure room available, start HFNC or bipap, as indicated.
- Alert airway team, if using in addition to your ED team members
- Admit to step-down or critical care unit
Applies to: Adult patients presenting to the emergency department with symptoms possibly related to COVID-19 infection, including fever, URI symptoms, respiratory symptoms, gastrointestinal symptoms, malaise, or fatigue.
This pathway is a guide and does NOT supersede good clinical judgment.
Figure 9.1. Evaluation Pathway for Suspected COVID-19



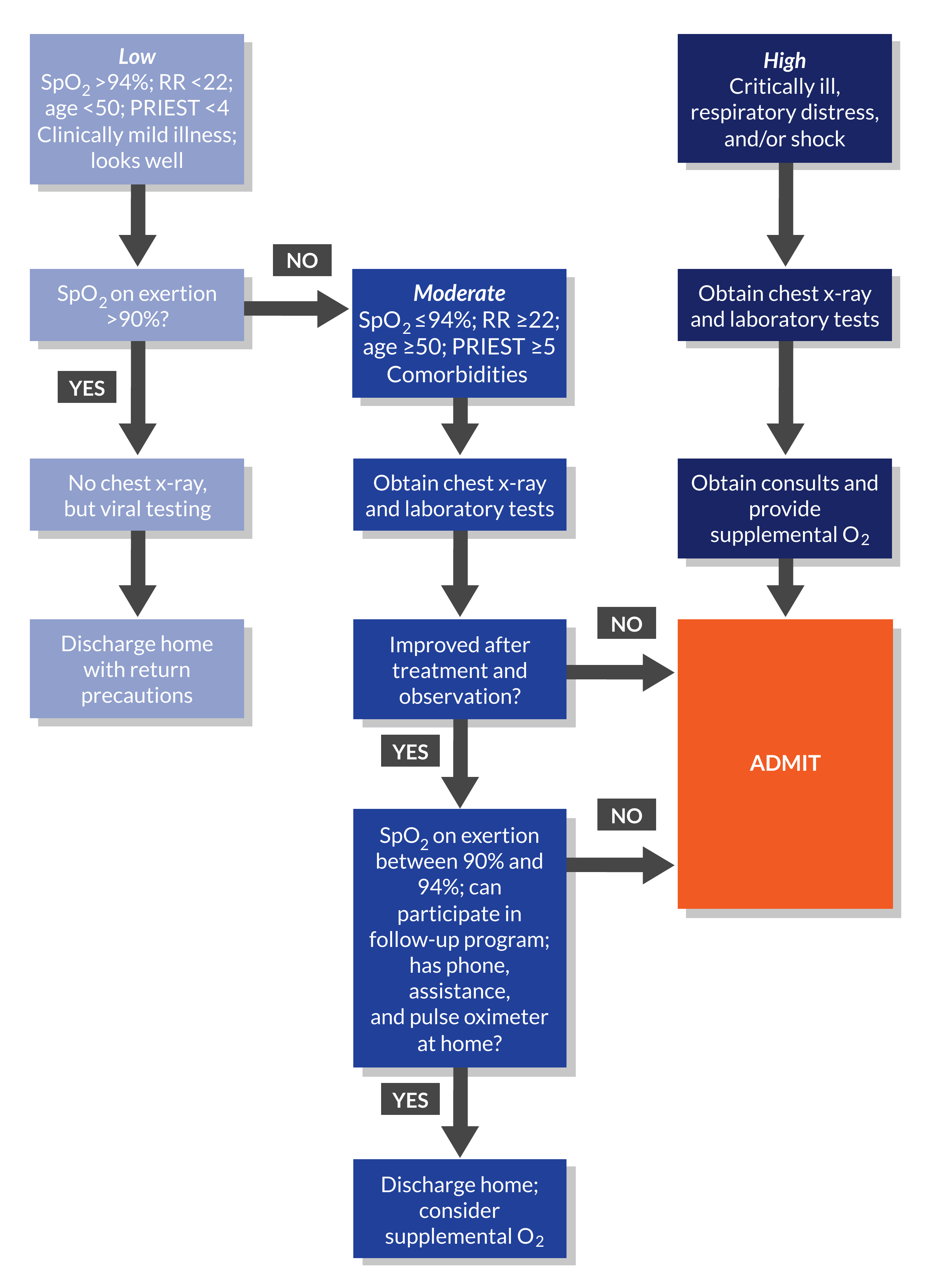
Figure 9.2 COVID-19 Screening Panel

References
- World Health Organization. Clinical management of severe acute respiratory infection (SARI) when COVID-19 disease is suspected. Published March 13, 2020.
- Alhazzani W, Møller MH, Arabi YM, et al. Surviving Sepsis Campaign: Guidelines on the Management of Critically Ill Adults with Coronavirus Disease 2019 (COVID-19). Intensive Care Med. 2020 Mar 28.
- Shi Y, Yu X, Zhao Het, al. Host susceptibility to severe COVID-19 and establishment of a host risk score: findings of 487 cases outside Wuhan. Critical Care. 2020 Mar 18;24(1):108.
- Yang J, Zheng Y, Gou X, et al. Prevalence of comorbidities in the novel Wuhan coronavirus (COVID-19) infection: a systematic review and meta-analysis. Int J Infect Dis. 2020 Mar 12;94:91-95.
- Zhou F, Yu T, Du R, et al. Clinical course and risk factors for mortality of adult inpatients with COVID-19 in Wuhan, China: a retrospective cohort study. Lancet. 2020 Mar 28;395(10229):1054-1062.
- Beeching NJ, Flectcher TE, Fowler R. Coronavirus disease 2019 (COVID-19). BMJ. April 2020.
- Carpenter CR, Mudd PA, West CP, et al. Diagnosing COVID‐19 in the Emergency Department: A Scoping Review of Clinical Examinations, Laboratory Tests, Imaging Accuracy, and Biases. Academic Emergency Medicine. 2020; 27:654– 670.
Thank you to Dr. Angela Mills, Dr. Rahul Sharma, and our New York Presbyterian Hospital leaders for their support while developing these guidelines.
Footnotes
†Department of Emergency Medicine, New York Presbyterian Hospital/Columbia University Irving Medical Center
‡Department of Emergency Medicine, New York Presbyterian Hospital/Weill Cornell Medical Center and Lower Manhattan Hospital
§Department of Emergency Medicine, New York Presbyterian Hospital/Brooklyn Methodist Hospital
||Department of Emergency Medicine, New York Presbyterian Hospital Queens
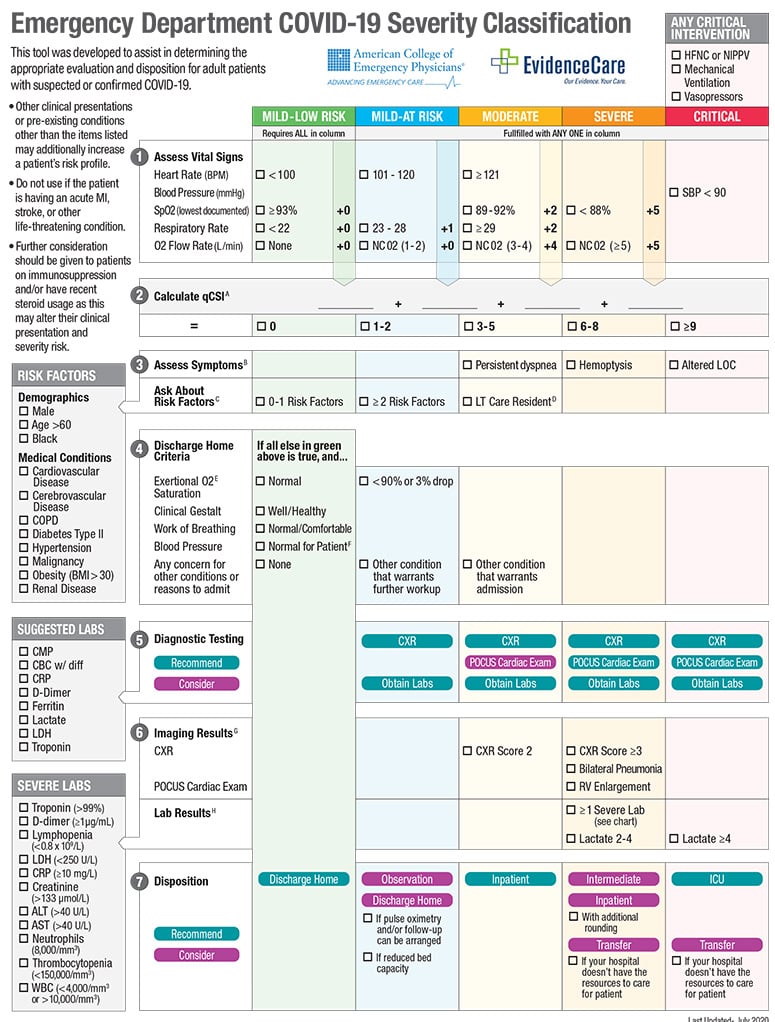
COVID-19 Severity Classification
ACEP and EvidenceCare created a seven-step triage process for emergency physicians to better classify COVID-19 patients and inform next steps. The new tool classifies patients on a range from mild/low risk to critical, based on seven categories of measurement: assessing vital signs, a qCSI calculator, symptoms and risk factors, discharge home criteria, diagnostic testing and suggested labs, imaging and lab results, and the disposition.
You can access the COVID-19 Severity Classification Tool in several ways –
- Link to the online interactive pathway at the Evidence Care website
- An integrated version for Epic, Cerner or T-Systems is also available. Hospitals can contact info@evidence.care for more information.
ACEP COVID19 Severity Classification Tool Contributors: Brian Fengler, MD - Co-Founder and Chief Medical Officer, EvidenceCare; Sandy Schneider, MD, FACEP - Associate Executive Director, ACEP; Amy Baxter, MD - CEO Pain Care Labs, Clinical Assoc. Prof Augusta University; Brenna Farmer, MD, MBA, MS - Site Director, New York Presbyterian Hospital Lower Manhattan Hospital ED; Director of Patient Safety, NYP/Weill Cornell Medical Center, Associate Professor of Clinical Emergency Medicine; Phil Parker, MD - GMO SCP-Health, SCP-Health; Jonathan A Handler, MD - Adjunct Associate Professor, Northwestern University Feinberg School of Medicine, Department of Emergency Medicine; Peter A D Steel, MA, MBBS - Director of Clinical Services, NYP/Weill Cornell Medicine Department of Emergency Medicine, New York Presbyterian Hospital-Weill Cornell Medicine; Amos J Shemesh, MD - Assistant Director of Clinical Services, NewYork-Presbyterian/Weill Cornell Medicine; Pawan Goyal, MD, MHA, FAMIA - Associate Executive Director, Quality, American College of Emergency Physicians; Sharon Hibay, DNP, RN - Chief Clinical Officer, Arch Systems, LLC; Christopher Corbit, MD, FACEP - Facility Medical Director, Summerville Medical Center; Tamara Moores Todd, MD; Todd B Taylor, MD, FACEP - Clinical Informaticist, Independent Consultant; Andrew S. Kanter, MD, MPH, FACMI, FAMIA - Chief Medical Officer, Intelligent Medical Objects; Edward H Suh, MD - Assistant Professor of Emergency Medicine, Columbia University Medical Center




