Author: Mark Hauswald, MS, MD, FACEP, Emeritus Professor of Emergency Medicine, Past Associate Dean for Clinical Affairs and Patient Safety, Past Director of Global Health Projects, University of New Mexico Health Sciences Center
The clinical presentation and progression of patients suspected of having COVID-19 can range from mild to severe. The laboratory workup for these patients is variable and depends significantly on each patient’s clinical presentation at the time of evaluation.
In patients with severe illness, the following tests should be ordered:
- CBC
- Comprehensive metabolic panel
Additional tests to consider include:
- ABG (as indicated to detect hypercarbia or acidosis);
- Coagulation screen;
- Inflammatory markers (serum procalcitonin [PCT] and C-reactive protein [CRP]);
- Ferritin;
- LDH;
- CK, CK-MB;
- Troponin;
- Blood and sputum cultures; and
- COVID PCR.
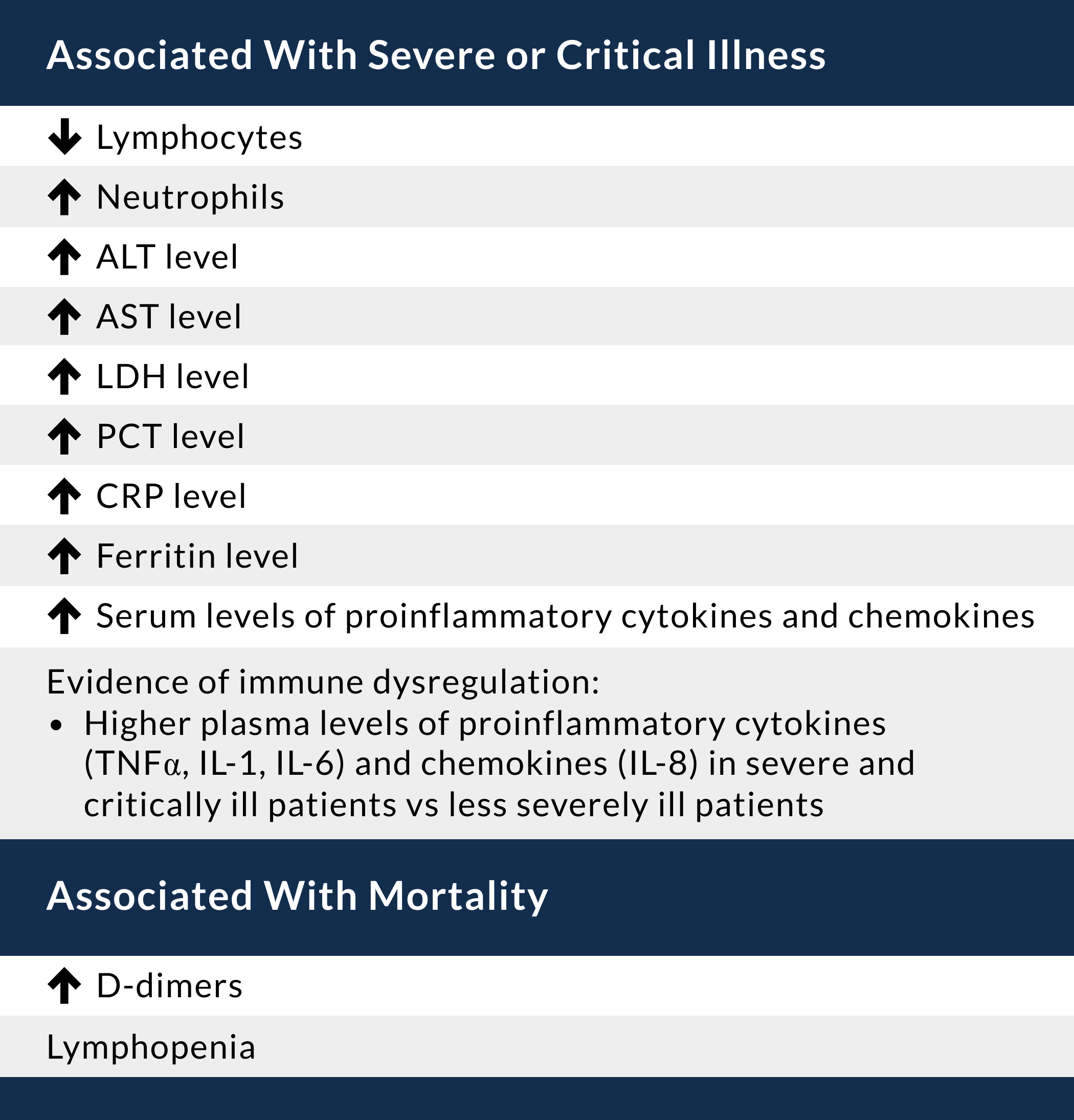
The most common laboratory abnormalities in patients hospitalized with pneumonia include leukopenia, lymphopenia, leukocytosis, elevated liver transaminases, elevated LDH, and elevated CRP (Table 9.1). Laboratory abnormalities in severe disease are further described in Table 9.2.
Table 9.1 Laboratory findings at hospital admission. Credit: ACEP.

Table 9.2 Laboratory abnormalities in severe disease. Credit: ACEP.
Hypercoagulability and COVID-19
Some patients with COVID-19 can develop signs of a hypercoagulable state and can be at an increased risk of venous and arterial thrombosis of large and small vessels. Laboratory abnormalities commonly observed in hospitalized patients with COVID-19–associated coagulopathy include:
- Mild thrombocytopenia;
- Increased D-dimer levels;
- Increased fibrin degradation products; and
- Prolonged PT.
Elevated D-dimer levels have been strongly associated with a greater risk of death.1-3
There have been several reports of hospitalized patients with thrombotic complications, most frequently deep venous thrombosis and pulmonary embolism.4,5 Other reported manifestations include:
- Microvascular thrombosis of the toes;
- Clotting of catheters;
- Myocardial injury with ST-segment elevation; and
- Large-vessel strokes.6-9
The pathogenesis of COVID-19–associated hypercoagulability remains unknown. However, hypoxia and systemic inflammation secondary to COVID-19 may lead to high levels of inflammatory cytokines and activation of the coagulation pathway.10 Limited data are available to inform clinical management of prophylaxis or treatment of venous thromboembolism in COVID-19 patients.
More information on hypercoagulability and COVID-19 is available from the American Society of Hematology’s “COVID-19 Resources” and the NIH’s “Antithrombotic Therapy in Patients With COVID-19.”
References
- Lippi G, Plebani M, Henry BM. Thrombocytopenia is associated with severe coronavirus disease 2019 (COVID-19) infections: a meta-analysis. Clin Chim Acta. 2020 Jul;506:145-148. doi:10.1016/j.cca.2020.03.022
- Lippi G, Favaloro EJ. D-dimer is associated with severity of coronavirus disease 2019 (COVID-19): a pooled analysis. Thromb Haemost. 2020;120(05):876-878. doi: 10.1055/s-0040-1709650
- Tang N, Li D, Wang X, Sun Z. Abnormal coagulation parameters are associated with poor prognosis in patients with novel coronavirus pneumonia. J Thromb Haemost. 2020 Feb 19;18:844-847. doi: 10.1111/jth.14768
- Klok FA, Kruip MJHA, van der Meer NJM, et al. Incidence of thrombotic complications in critically ill ICU patients with COVID-19. Thrombosis Research. 2020 Jul;191:145-147. doi: 10.1016/j.thromres.2020.04.013
- Helms J, Tacquard C, Severac F, et al; CRICS TRIGGERSEP Group. High risk of thrombosis in patients in severe SARS-CoV-2 infection: a multicenter prospective cohort study. Intensive Care Med. 2020 Apr;46(6):1089-1098. doi: 10.1007/s00134-020-06062-x
- Grillet F, Behr J, Calame H, et al. Acute pulmonary embolism associated with COVID-19 pneumonia detected by pulmonary CT angiography. Radiology. 2020 Sep;296(3). doi: 10.1148/radiol.2020201544
- Oxley T, Mocco J, Majidi S, et al. Large-vessel stroke as a presenting feature of COVID-19 in the young. NEJM. 2020 Apr;382:e60. doi: 10.1056/NEJMc2009787
- Avula A, Nalleballe K, Narula N, et al. COVID-19 presenting as stroke. Brain Behav Immun. 2020 Jul;87:115-119. doi:10.1016/j.bbi.2020.04.077
- Margo C, Mulvey J, Berlin D, et al. Complement associated microvascular injury and thrombosis in the pathogenesis of severe COVID-19 infection: a report of five cases. Transl Res. 2020 Jun;220:1-13. doi: 10.1016/j.trsl.2020.04.007
- Bangalore, S; Sharma, A; Slotwiner, A et al. ST-segment elevation in patients with COVID-19 — a case series. NEJM. 2020 Apr 17. doi: 10.1056/NEJMc2009020
Additional readings
- Huang C, Wang Y, Li X, et al. Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China. Lancet. 2020 Feb 15;395(10223):497-506. doi:10.1016/S0140-6736(20)30183-5
- Chen N, Zhou M, Dong X, et al. Epidemiological and clinical characteristics of 99 cases of 2019 novel coronavirus pneumonia in Wuhan, China: a descriptive study. Lancet. 2020 Feb 15;395(10223):507-513. doi:10.1016/S0140-6736(20)30211-7
- Wang D, Hu B, Hu C, et al. Clinical characteristics of 138 hospitalized patients with 2019 novel coronavirus-infected pneumonia in Wuhan, China. JAMA. 2020 Feb 7;323(11):1061-1069. doi:10.1001/jama.2020.1585

