ACEP ID:
- My Account
- My CME
- Sign Out
ACEP ID:
Steady increases in medical school tuition and living expenses for medical students have resulted in high levels of graduating student indebtedness, a matter of concern to the Association of American Medical Colleges (AAMC) and many specialty society organizations, including the American College of Emergency Physicians (ACEP), and to resident organizations, including the Emergency Medicine Residents' Association (EMRA).
In response to this concern, ACEP's Academic Affairs Committee (AAC), in collaboration with EMRA, developed a module, the "Medical School Debt/Loan Repayment-Forgiveness." The subcommittee reviewed (and borrowed extensively from) the AAMC's "Report on Medical School Indebtedness" 2004 publication, and other sources during the preparation of this report.
In addition, we offer suggestions for ACEP to consider on how to respond in a meaningful manner to the level of medical student indebtedness and the burdens the debt and its repayment place on medical students, residents, and young physicians. We also provide preliminary information on current programs that are available to address medical education debt and loan repayment forgiveness for resident trainees.
ACEP staff met with the leadership of the National Health Service Corps (NHSC) in September 2006 to ascertain if there is a demand for emergency physicians (EPs) in underserved areas. The NHSC has always been focused on providing primary/outpatient care to underserved areas/populations. Under-service is characterized by Health Professions Shortage Area (HPSA) designations that are generated from physician/population ratios. The Public Health Act (PHA) is the controlling statute for HPSA designation and NHSC and explicitly identifies family medicine, obstetrics/gynecology (OB/GYN), and general pediatrics, internal medicine, and psychiatry as eligible physician specialties. This means that the law would have to be changed to add emergency medicine to the list of physicians eligible for scholarship and loan repayment. Less than 4,000 clinicians are currently supported by NHSC, which includes nurses, counselors, dentists, and other health care personnel.
While the American Hospital Association's (AHA) Small and Rural hospital section director stated that members would welcome more board-certified emergency physicians, the NHSC physicians generally become employees of the Federally Qualified Health Clinics or set up private, office-based practices subsidized by the communities. In recent years, NHSC's annual budget has remained fairly stable at $125M. The funds have been shifted to loan repayment while scholarship dollars have dwindled and are largely directed to racial/ethnic minorities. NHSC requires a minimum 2-year commitment in order to receive partial debt relief, though many clinicians remain for five years in order to receive full loan forgiveness.
ACEP's Public Affairs staff have monitored the provisions of the PHA (including NHSC and HPSA designation criteria) as they came up for reauthorization in 2007. Lobbying efforts to include emergency medicine as a primary care specialty eligible for NHSC funding have not been successful. Continued efforts to lobby for this designation are limited by available NHSC funding, attempts of multiple other specialties trying to qualify for primary care loan reimbursement, and other high priority issues (access to care, overcrowding, etc.) with limited time and resources available for lobbying.
To obtain more information/data on the need and demand for EPs in rural or underserved areas, subcommittee members and ACEP staff have contacted members of the ACEP's Rural Section and other organizations such as the Rural Appalachian Organization, and the National Rural Health Association.
From the supply side, in 2006, EMRA conducted a resident survey to obtain information on EM residents' interest in loan forgiveness programs and their willingness to work in rural and underserved areas. The Council for Emergency Medicine Residency Directors (CORD) also conducted a survey on program interest in rural EM and support for resident electives in rural EM. Results of EMRA's survey are noted below.
Are you interested in rural emergency medicine?
Yes - 232
No - 82
Would you consider a job in a rural location if loan repayment was an incentive?
Yes -274
No -39
Would you consider taking a job in a rural location if loan repayment was not an option?
Yes -162
No - 152
Do you feel advocating for residency education in rural environments is as important an issue as other advocacy issues like overcrowding and medical liability?
Yes - 213
No -100
I would like to work with EMRA on Rural Emergency Medicine Initiatives
Yes -80
No -212
Narrative Comments (representative of more than 50 provided):
"Emergency medicine IS primary care (no one refers the patient to us!) It should have the same incentives as other fields of primary care, such as loan repayment for practice in underserved areas."
"A large percentage of the population is receiving care from ED physicians who are not residency trained. ACEP should be making real efforts to encourage residency trained physicians to look at opportunities in rural areas, and loan repayments are a great way to start."
"I would consider rural emergency medicine without the incentive, but much more likely to take a job with the incentive (of loan repayment). I'm from a small town, and would love to go back…"
"I have rotated in rural internal medicine during 3rd year med school and would definitely consider working there at least part time after I finish residency. Loan repayment for ED in rural areas is an absolute necessity as these facilities are grossly understaffed."
"I would definitely serve in a rural area if loan forgiveness was provided."
"I cannot stress more the need for modern, competent and compassionate emergency care in the rural setting. We all seem to recognize the need in the dense urban populations, but fail to remember that the rural poor suffer from inadequate preventative care as well. Unfortunately, there seems the need for some incentive to care for this population in order to offer the clinician a competitive place in the field."
ACEP, the Society for Academic Emergency Medicine (SAEM), and the Association of Academic Chairs of Emergency Medicine (AACEM) have all emphasized the importance of reimbursement for residency programs before programs could consider implementing rural EM residency training. In September 2006, ACEP President Frederick C. Blum, MD, FACEP, FAAP, sent a letter to the three organizations updating them on ACEP's continued efforts to address a council resolution relating to this issue.
Other advocacy activities have also been initiated by ACEP. In June 2006, ACEP sent a letter to the Centers for Medicare and Medicaid Services (CMS) in response to its proposed changes to the hospital inpatient prospective payment system. Unfortunately, CMS subsequently determined that ED rotations away from the parent institution will not be allowed to be credited in the parent institutions accounting of resident service for which the parent institution may receive Medicare GME funding, thus the barrier to rotations in rural ED settings still exists for the vast majority of training programs. On March 22, 2007, ACEP submitted a follow up response to this decision to the CMS leadership in a continued effort to convince them to change their interpretation of the allocation of Medicare GME funds to parent institutions for away ED clinical rotations. This change, if implemented, would eliminate a major financial barrier for programs that choose to provide residents with rural EM training experience(s).
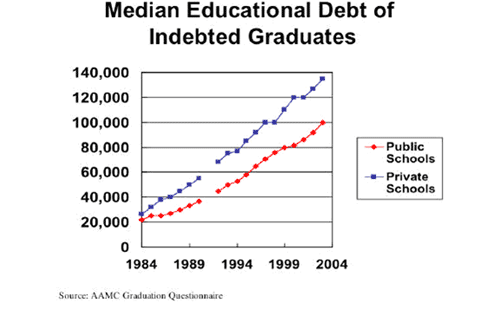
© 2004 Association of American Medical Colleges. Medical School Tuition and Young Physician Indebtedness. All rights reserved.
Reproduced with permission of the Association of American Medical Colleges.
Data from the AAMC Matriculating Student Questionnaire demonstrate that student expectations for financing their medical education have shifted substantially toward loans and scholarships (see figure below). In 1987, the average student expected to pay 40.5% of the cost of his or her medical education from family, personal, and other sources, with the balance from loans and scholarship. By 2003, expectations of support from family, personal and other sources had all substantially declined, with the aggregate percentage for these sources reduced to 21.5%. This change is an indication that the cost of a medical education is becoming more difficult for students and their families.
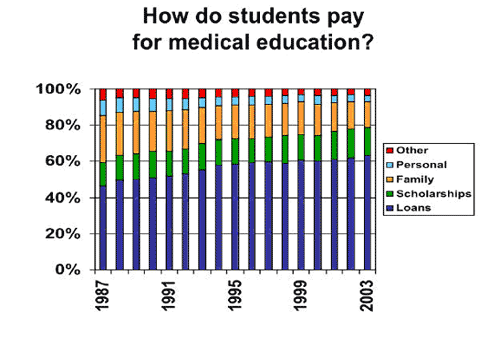
© 2004 Association of American Medical Colleges. Medical School Tuition and Young Physician Indebtedness. All rights reserved.
Reproduced with permission of the Association of American Medical Colleges.
A. Medical school-provided scholarships are significant
Scholarships are a significant help to students in coping with the cost of medical school attendance, amounting to 28% of tuition costs in public schools and 27% of tuition costs in private schools in 2002. For students in public medical schools, tuition costs are lower than in private schools, but the other costs of attendance are roughly the same. Because scholarships provide only 12% of the total costs of attendance in public schools versus 18% of the total costs in private schools, the total debt of private school students is not as large as the initial difference in tuition would suggest.
B. Non-medical school-provided scholarships available to students
The following states informed a subcommittee member that there was no loan forgiveness program for EM physicians currently in a residency training program: Alabama, Idaho, Illinois, Kentucky, Missouri, Nebraska, South Dakota, Virginia, West Virginia, and Wisconsin.
There are a variety of loan programs available to medical students that provide ample funds under very favorable terms. Students can borrow up to $8,500 per year under the federally subsidized Stafford loan program, and they can increase the amount to $38,500 per year on an unsubsidized basis. The (2003) interest rate on the unsubsidized Stafford loans is at or near historic lows at 2.82%. When combined with undergraduate Stafford indebtedness, the total borrowing limit for Stafford loans is $189,125, and students have ten years to repay. Additional borrowing is available under alternative loan programs like MEDLOANS at 4%, with up to 20 years to repay. In general, loans are readily available to medical students at favorable terms, though loan debt exceeding the $189K limit will need to be covered by more traditional lending institutions at a much higher rate.
Traditionally, many of the state and federal loan programs deferred interest and/or repayment schedules until after completion of internship, though many of these programs require an economic hardship means testing in order to qualify past the internship year. In April 2007, the AAMC endorsed the "Medical Education Affordability Act," a bill proposed in the U.S. Senate that would allow physicians to defer repayment of their student loans while they complete their residency or fellowship training. Current law relating to the economic hardship deferment option allows physicians who meet specific debt-to-income ratios to defer repayment of federal educational loans for up to three years. The new proposed legislation would extend this deferment to include the entire length of "postgraduate medical or dental internship, residency, or fellowship programs." More than 20 additional medical and dental associations and organizations have also endorsed the bill.
Physician incomes are high compared to most occupations, allowing repayment of even relatively high levels of debt, once a practice is established. The estimated median physician income in 2003 was $187,600, a figure that is close to that of the emergency medicine community for the same year. Appreciate that in recent years, however, physician incomes have increased only slowly, and in constant dollars the amounts have trended slightly downward.
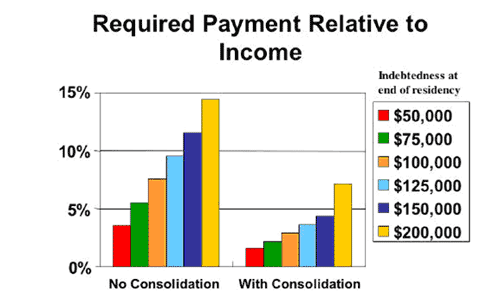
© 2004 Association of American Medical Colleges. Medical School Tuition and Young Physician Indebtedness. All rights reserved.
Reproduced with permission of the Association of American Medical Colleges.
Since 1990, median physician income has increased by 34.6%, almost exactly in line with consumer prices. Since medical graduate indebtedness has increased much more rapidly, repayment of educational loans is clearly more difficult today than it has ever been. With current median physician income levels, repayment of debt at levels common today could become very burdensome unless consolidation is employed. Consolidation allows the borrower to combine all federal loans in one package at a blended rate of interest, and to stretch out payments for up to thirty years. (See figure above)
ACEP should research and make available to all emergency medicine residents information regarding financial aid programs to lessen the financial burden of their medical education. ACEP should take a leadership role in supporting and promulgating efforts at the local, state, and national levels, to assist other organizations and governmental bodies in the development of financial aid programs to emergency medicine residents. Whenever possible, these programs should dovetail with efforts to address health care needs of medically underserved populations of society, particularly in inner city and rural areas of our country.
Specific ACEP activities might include:
Medical Educational Costs and Student Debt: A Working Group Report to the AAMC Governance. Association of American Medical Colleges, 2005
Jolly P: Medical School Tuition and Young Physician Indebtedness. Association of American Medical Colleges, March 23, 2004
Ankle, Felix. Memorandum: Rural Emergency Medicine Workforce. The ACEP AAC Subcommittee on the Rural EM Workforce, September 20, 2006.
Submitted May 2007 by Academic Affairs Committee:
John J. Kelly, DO, FACEP, Committee Chair
David S. Howes, MD, FACEP, Subcommittee Chair
Gillian Schmitz, MD, EMRA Board of Directors
Felix K. Ankel, MD, FACEP
Jonathan Fisher, MD, FACEP
Adam C Ouimet, MD
Nick Kestner, Chapter Executive