ACEP ID:
- My Account
- My CME
- Sign Out
ACEP ID:
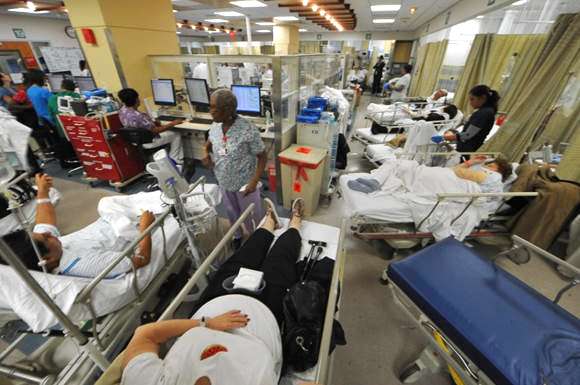
Feel overcrowded? Need more inpatient beds, nurses? Do you realize you may be hemorrhaging millions because of FIXABLE problems with flow and length of stay? Don’t add a single bed or staff member until attending this conference. Maybe you won't need any.
There are 100’s of process improvements for flow, but only a handful actually work to FIX problems associated with an apparent lack of sufficient inpatient beds. Before you launch another initiative or hire another consultant, learn about the key processes that work (and ones that don’t), with practical advice from hospital experts with first-hand experience.
Join the leaders in hospital flow at the Innovation Leadership Challenge: Collaborating to Improve Hospital Flow, Save Lives and Reduce Costs pre-conference which offers battle-tested solutions so you can:
Don’t waste your time with ineffective solutions. This conference focuses on the true “home runs” of flow improvement, with real life examples and practical advice. Adopting the practices described in this conference will reduce or entirely eliminate boarding, free up beds and staff, improve throughput, enhance patient satisfaction and safety, and sharply reduce costs.
Make plans to join us, so you can begin to make dramatic improvements in capacity and patient safety, all with decreased costs to your hospital. Included in this activity are practical workshops that will help the participants move from “what” to “how to make it happen”.
The Innovation Leadership Challenge: Collaborating to Improve Hospital Flow, Save Lives and Reduce Costs is a pre-conference event at the American Hospital Association Leadership Summit.


|
8:00 am – 8:10 am |
Introduction Jay Kaplan, MD, FACEP |
|
8:10 am – 8:30 am |
Keynote Jay Bhatt, DO, MPA, FACP |
|
8:30 am – 8:40 am |
Design Thinking and Instructions for the Day
Andrew Shin, JD, MPH |
|
8:40 am – 9:30 am |
Introduction to the Problem
Peter Viccellio, MD What happens when we’re crowded, and what works to fix it? The speaker will discuss the following points:
|
|
9:30 am – 9:45 am |
Break |
|
9:45 am– 11:30 am |
Smoothing of Elective Admissions
John Chessare, MD What drives capacity problems? The speaker will discuss the following points:
|
|
11:30 am – 12:30 pm |
Lunch |
|
12:30 pm – 1:00 pm |
Full Capacity Protocol Carolyn Santora, RN
|
|
1:00 pm – 1:30 pm |
Enhancing Weekend Discharges
Peter Viccellio, MD How does discharge activity on the weekend impact on capacity? The speaker will discuss the following points:
|
| 1:30 pm – 2:00 pm | Early Discharge
Jay Kaplan, MD, FACEP How does inpatient discharge time impact on capacity? The speaker will discuss the following points:
|
| 2:00 pm – 2:15 pm | Break |
| 2:15 pm – 3:30 pm |
Table Design Exercise Each table developing strategies to engage leaders across their health care organizations in improving and optimizing hospital flow. Teams will use design canvases to co-create strategies and innovative ideas in a systematic way to produce real results. |
| 3:30 pm – 4:30 pm |
Table Report Out The groups will share their successful approaches. |
|
4:30 – 4:45 pm |
Wrap-up Session |