Case Study of the Month- Chest Pain in a 16-Year-Old
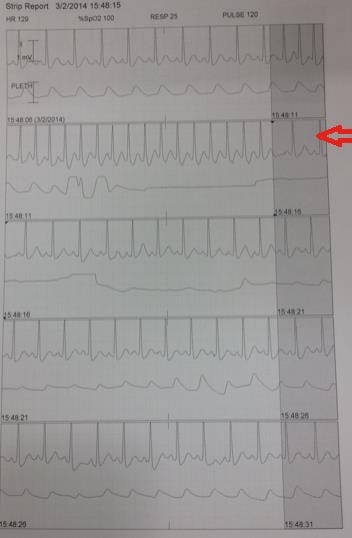
A 16-year-old morbidly obese female presents to the ED with breathing difficulty, chest pain, and wheezing for the past 30 minutes. She denies any prior history of asthma, but states that she was treated and released from the hospital one day earlier for an acute allergic reaction to an unknown agent. Today’s episode occurred suddenly, and the patient states that she was sitting on the couch when her symptoms began. She denies any known allergies, and reports no other medical history. She is noted to have very poor air entry in both lung fields and is in obvious distress. Anaphylaxis treatment pathway is initiated. A few minutes later, she reports intermittent sharp stabbing pain in her chest, lasting 8-10 seconds each time. The following rhythm is noted on the monitor, and corresponds with her acute pain episodes.
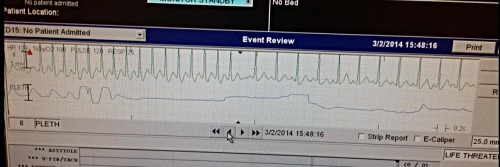
Physical exam
The patient has the following vitals:
- T 37.1 oC HR 120 RR 25 BP144/92
- Pulse ox: 100% on 2L O2 by NC (97% on room air)
- Weight: 136.2 kg
- General: Alert,but anxious, slightly diaphoretic. Capillary refill <2 seconds, distal pulses intact.
- Cardiovascular: S1, S2, Rate regular, no murmurs, gallops, rubs
- Respiratory: Prolonged expiration, I/E wheezes throughout the lung fields.
Rest of the examination is unremarkable. Over the next 10 minutes, the rhythm noted below continues to occur every 2-3 minutes, and lasts 8-10 seconds. Each time, the patient experiences severe chest pain during the episode.