1st Place Emage Winner: Fragile Skin, Be Careful: Acute Management of Epidermolysis Bullosa
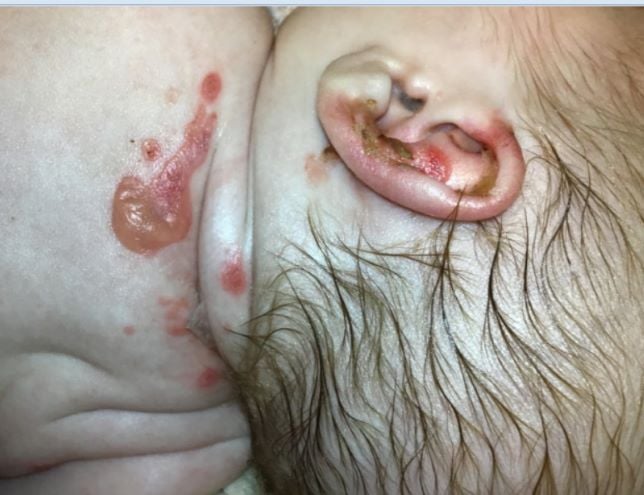
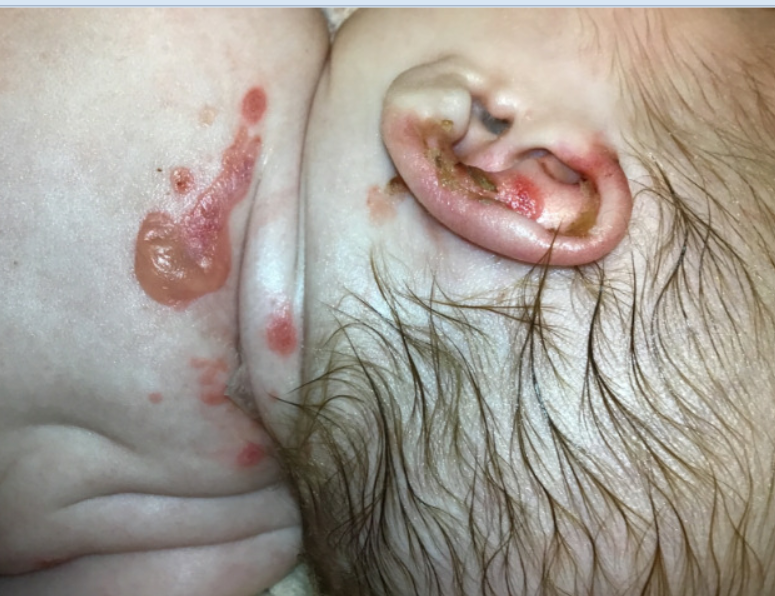
A 4-week-old female with junctional epidermolysis bullosa (JEB) diagnosed at birth presents with worsening skin irritation in the setting of vomiting and diarrhea. For a week leading up to presentation, parents noticed increased skin redness, peeling, and malodorous smell from wounds due to frequent diarrhea and diaper changes.
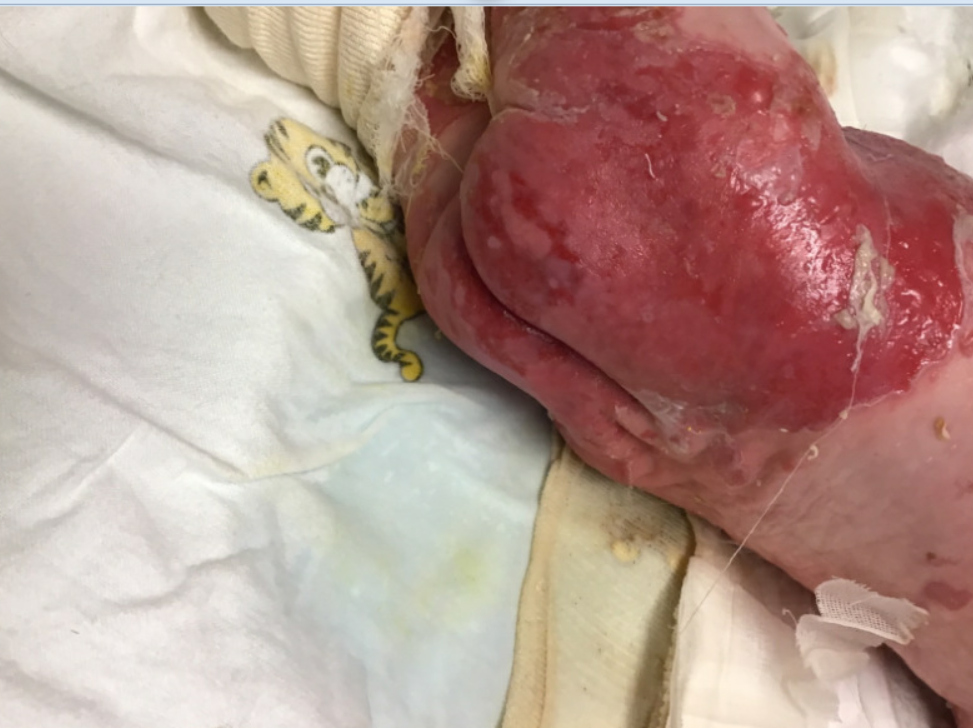
JEB is a subtype of epidermolysis bullosa, a rare genetic connective tissue disorder characterized by excessive fragility of the skin.1 As the diagnosis of JEB in this patient had been already established prior to presentation, the purpose of this case report is to discuss skin care and management of infants with EB in emergency settings.
Our patient presented with a history typical of gastroenteritis, which is common and usually uncomplicated in the pediatric population. However, the patient’s fragile skin and open wounds placed her at higher risk for infection and water loss. Management is also more challenging due to the necessity of sensitive and careful handling of the patient. Common medical practices, such as intravenous (IV) line placements, blood pressure, and pulse ox measurements, are all traumatic to her skin and induce bullae formation; therefore, dermatology was immediately consulted for recommendations on how to appropriately handle the patient.

Avoiding friction and shearing forces as much as possible is critical in patients with EB.2 While pressure/compressive forces may also damage the skin, they are more tolerable and less damaging than frictional and shearing forces.2 Therefore, obtaining initial blood pressure (BP) via a manual cuff and limiting re-measurements was recommended.
While our patient’s vitals, PO (by mouth) intake, and hydration status were reassuring, we had to obtain IV access for labs, maintenance fluids, and antibiotics due to suspicion for possible cellulitis. Avoiding adhesives is critical to limiting skin damage. Securing the IV in this case was achieved by wrapping Vaseline and cotton gauze around the line. Tape can be applied over the dressing, but not directly on the skin.2
To further protect the skin and promote healing, keeping the patient’s skin lubricated was achieved with Vaseline, zinc oxide creams, and antibiotic ointments. Open wounds should always be dressed. A common recommended practice is the application of three layers; the first or primary layer is non-adherent, the second layer stabilizes the primary layer and provides padding and protection. The third layer is used to maintain the dressing in place. It is usually somewhat elastic in nature.1 For our patient, we used Vaseline gauze, followed by a layer of absorptive cotton padding, then wrapped with Kerlix. Nurses and providers examining the patient were also recommended to apply Vaseline on their gloves to further limit friction.
After proper vital sign measurement, wound care, IV placement and fluid administration, our patient was started on IV Cefazolin due to concern for cellulitis and was transitioned to the pediatric intensive care unit (PICU). Further recommendation by dermatology included application of gentamicin 0.5% ointment BID. While laminin 332 is mutated in JEB due to a premature stop codon, gentamicin is known to allow read through of this premature stop codon and allow for partial restoration of the normal protein product, which may assist in wound healing.3
References
- Epidermolysis bullosa (EB) How to. How To | debra of America. (n.d.). Accessed July 31, 2022. https://www.debra.org/how-to
- Saraf SV, Mandawade NJ, Gore SK, Padhye UD, Pereira CS. Epidermolysis bullosa: Careful monitoring and no touch principle for anesthesia management. J Anaesthesiol Clin Pharmacol. 2013 Jul;29(3):390-3. doi: 10.4103/0970-9185.117112.
- Kwong A, Cogan J, Hou Y, Antaya R, Hao M, Kim G, Lincoln V, Chen Q, Woodley DT, Chen M. Gentamicin Induces Laminin 332 and Improves Wound Healing in Junctional Epidermolysis Bullosa Patients with Nonsense Mutations. Mol Ther. 2020 May 6;28(5):1327-1338. doi: 10.1016/j.ymthe.2020.03.006.
Dalia Ishaq, MD1
Mary Elizabeth Bernardin, MD2
1: Department of Child Health, University of Missouri School of Medicine, Columbia, MO
2: Division of Pediatric Emergency Medicine, Department of Emergency Medicine, University of Missouri School of Medicine, Columbia, MO