

The Geriatric Emergency Department Accreditation (GEDA) program is an ACEP-governed national accreditation organization which strives to improve the care of older adults presenting to the emergency department. This accreditation system promotes the goals quality of care for older people: enhanced staffing and education; geriatric-focused policies and protocols including transitions of care; quality improvement and metrics; and optimal preparation of the physical environment.
The following criteria outline the minimum standards for accreditation of a Geriatric Emergency Department in three levels.
Level 3 accreditation is represented by one or more geriatric-specific initiatives that are reasonably expected to elevate the level of elder care in one or more specific areas. Additionally, personnel to implement these efforts are identified and trained.
Level 2 accreditation identifies sites that have integrated older adult initiatives into daily operations. They demonstrate interdisciplinary cooperation for delivery of senior-friendly services. They have an established supervisor or director coordinating the people who are tasked with the daily performance of these services.
Level 1 accreditation defines an ED with a comprehensive care system in place for improving the care of older adults, including but not limited to: senior-specific policies, guidelines, procedures, interdisciplinary staff (both within the ED and throughout the institution), outcome measurements and evaluation efforts. Additionally, they may have physical facility enhancements designed to improve older adult care.
Current online application fees:
Level 1: $15,000 Level 2: $7,500 Level 3: $2,500Level 1 requires a site visit and a reviewer can request a site visit for Level 2. Applicants are responsible for arranging and reimbursing the site visitor for travel, lodging and expenses related to the visit. Accreditation will be granted for 3 years.
This guide book contains several chapters relevant to accreditation: Creating a Geriatric Emergency Department, published by Cambridge University Press, is available from Amazon.
Please contact Nicole Tidwell at ntidwell@acep.org for instructions on how to easily submit multiple applications.
Once you have submitted a completed application, it will be reviewed by two ACEP-appointed expert geriatric emergency physicians. You may be asked additional questions to clarify parts of your application. If you are applying for a Level 1 geriatric ED, a one-day site visit will be required. If you are applying for a Level 2 geriatric ED and there are questions about your application, then you may be asked to arrange a one-day site visit. Level 3 accreditation does not require a site visit.
Following the site visits, if needed, your application must be approved by the GEDA Board of Governors. The entire process is anticipated to take approximately 10-12 weeks, depending on application level.
In addition to the application itself, there are a number of documents that will be required to complete your application. You can visit the Getting Started page for a list of sample documents to get you started.
Please review the sample documents page and gather these required elements before starting your online application.
Use of Telehealth to meet Level 1 & 2 GEDA Requirements
Geriatric Emergency Medicine places a strong emphasis on interdisciplinary teamwork, and this is reflected in the GEDA requirements for accredited Geriatric EDs. In particular, the GEDA requirements for Level 1 & 2 GEDs include many of the following for each applying ED: 56 hours case management/ social work coverage per week in the ED, medication management/ pharmacy coverage, physical therapy, and occupational therapy. However, many EDs that seek (or may seek) GEDA Level 1 or 2 recognition are smaller and/ or rural EDs where it is unlikely that many of these services can be based in the ED due to the fewer number of patients needing their services at any one time. As such, it may make sense for these EDs to use telehealth to provide these interdisciplinary services. As an alternative platform for care delivery, Telehealth has gained traction in many clinical domains across multiple specialties including emergency medicine. Given that little is currently known about the efficacy of telehealth to provide these interdisciplinary services, this toolbox is provided to set guidelines for how EDs might consider the use of telehealth to meet these GEDA application requirements. GEDA recognizes and supports the use of telemedicine to address certain services that are not currently available.
The GEDA Upgrade Program is available to any Level 2 or Level 3 site that wishes to achieve a higher level of accreditation within their current award period. If you are upgrading at least 120 days prior to your current accreditation award expiration, the fee paid with your accreditation award will count towards your upgrade (if the upgrade takes place within the accreditation term of 2.6 years.)
Yes! Read about Geriatric Emergency Departments (PDF). Reproduced with permission from ACEP’s Emergency Department Design: A Practical Guide to Planning for the Future, 2nd Ed., by Jon Huddy, AIA
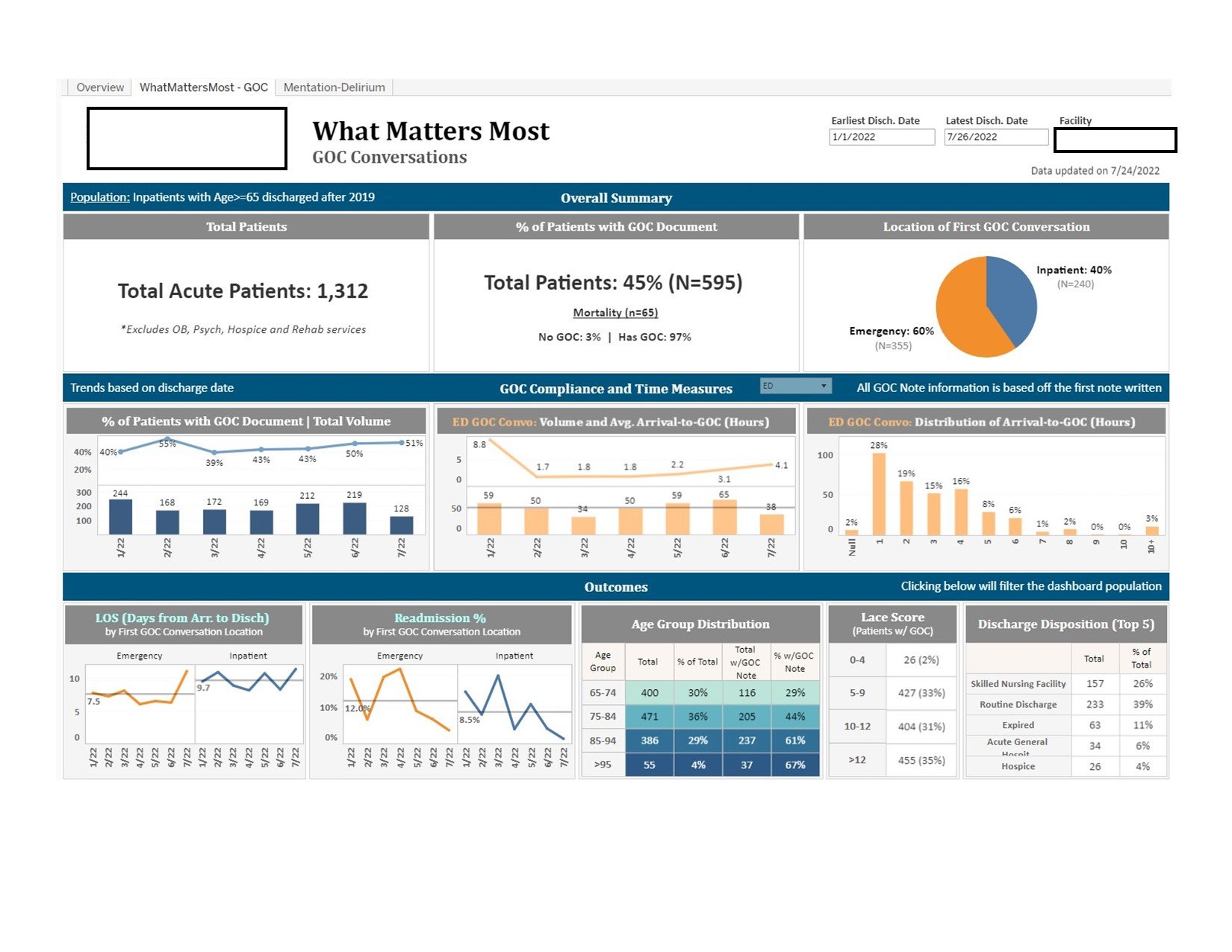
Level 1 and Level 2 sites should submit a process map/workflow of their GED process flow showing the standardized approach to care process completion (who does the care processes and when they are done). Level 1 sites must also submit a copy of their GED dashboard showing how they track and monitor execution of the relevant care processes. See examples:
In collaboration with the Geriatric Emergency Department Collaborative and the Indian Health Service the following assets are available.
Rural Hospital Geriatric Emergency Toolkit. The toolkit includes resources curated for rural and remote EDs, education resources, low-barrier interventions recommended by clinicians working in rural settings.
Indian Health Service GED’s, Alzheimer’s and Dementia work
Geriatric Emergency Department Accreditation (GEDA) | Alzheimer's Disease and Dementia Program
Know and align care with each older adult’s specific health outcome goals and care preferences including, but not limited to, end-of-life care, and across settings of care.
If medication is necessary, use Age-Friendly medication that does not interfere with What Matters to the older adult, Mobility, or Mentation across settings of care.
Prevent, identify, treat, and manage dementia, depression, and delirium across settings of care.
Ensure that older adults move safely every day in order to maintain function and do What Matters.
An initiative of The John A. Hartford Foundation and the Institutue for Healthcare Improvement (IHI) in partnership with the American Hospital Association (AHA) and the Catholic Health Association of the United States (CHA).