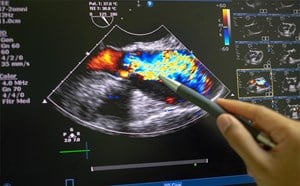
Extending Point-of-Care Ultrasound to Spaceflight Environments: Implications, Challenges and Workshop Innovation
*cover photo: Group shot of our OSMED (Organization for Space Medicine, Engineering, and Design)
Chanel Fischetti, MD
Introduction
As human spaceflight evolves and missions extend in duration, destination and complexity, medical care aboard spacecraft or in extraterrestrial habitats must adapt. Among imaging modalities, point-of-care ultrasound (POCUS) presents a uniquely optimal tool for microgravity due to its portability, low‐mass, and diagnostic ability without radiation.1
Why Ultrasound in Space?
In the microgravity environment, physiology changes dramatically—fluids shift, muscles and bones atrophy, and cardiovascular adaptation occurs. The ability to visualize anatomy and function in real time offers a critical advantage for diagnosis and treatment when resources are limited.
POCUS meets the unique demands of space medicine through:
- Compact design and efficiency: Ultrasound units are light, require minimal power, and occupy little volume, ideal for spacecraft and low-resource settings.1
- Versatile diagnostics: From cardiac and pulmonary evaluation to musculoskeletal injury and neuro-ocular changes, POCUS offers dynamic imaging for a variety of organ systems.2
- Crew autonomy: During deep-space missions, communication delays make it impossible to rely on real-time terrestrial consultation. Structured training is therefore critical both for independent image acquisition and interpretation.1
From Earth to Orbit: Key Considerations for Space POCUS
1. Training & Competency
Unlike terrestrial hospitals, space crews may include non-physician medical officers or engineers serving as “technician-operators.” Training must therefore emphasize probe handling, image acquisition, interpretation, and clinical decision-making. Although artificial intelligence (AI) may eventually support automated image acquisition or interpretation for novice users, it cannot replace the value of hands-on training or the foundational knowledge and technical skills required for competent image acquisition. Workshops and simulation-based practice are vital for skill retention and confidence. Emerging frameworks, including proposed competency-based curricula for “Spaceflight POCUS” (SPOCUS), lay the groundwork for standardized astronaut training.1,3
2. Equipment and Operational Challenges in Microgravity
In the absence of gravity, proper positioning of both the operator and the subject is challenging, often necessitating restraint with straps or Velcro. Traditional coupling gel may float away or bubble, so alternatives such as water or gel pads are being explored.1 Hardware must withstand radiation, vibration, and temperature fluctuations while remaining serviceable with limited repair options. Every gram and watt counts, so devices must balance durability and diagnostic performance.4
3. Clinical Applications and Limitations
SPOCUS can support a broad range of evaluations, including deep vein thrombosis detection, pulmonary assessments (B-lines, pneumothorax), ocular exams (optic nerve sheath diameter), musculoskeletal injuries, renal and bladder scans, and trauma assessment.1,3
However, microgravity alters baseline physiology: fluids redistribute, organs shift, and acoustic windows change, potentially modifying image interpretation. Tele-ultrasound consultation from Earth can help, but latency and bandwidth limitations may restrict dynamic feedback, underscoring the importance of autonomous crew training.2
4. Image Quality, Storage, and Decision Support
On Earth, image review and quality assurance are routine. In orbit, data transmission is limited by bandwidth, so AI-driven or on-board review tools could bridge this gap. Automated feedback on image quality, diagnostic flags, and storage optimization will likely play a major role in future missions.5,6
5. Future Directions
Space ultrasound research is evolving rapidly. As experience grows, formalized SPOCUS curricula and performance standards will help ensure consistency and safety across crews.1 Additionally, further research in longer-duration missions is needed to validate POCUS protocols, diagnostic yield, and their impact on mission safety and outcomes. Augmented and mixed-reality systems, such as HoloPOCUS,7 may guide probe placement or display anatomy overlays in real time. “Just-in-time” refreshers and interactive training modules could help maintain skills during long missions.1,3
Hands-On in Hawaii: The OSMED “Space POCUS” Workshop
At the inaugural Organization for Space Medicine, Engineering, and Design (OSMED) Conference in Maui, Hawaii, participants experienced the first-ever hands-on Spaceflight POCUS (SPOCUS) workshop, marking a new chapter in space medicine education.
The course paired a keynote lecture on the evolution of ultrasound in space with an immersive practical session led by experts in both clinical and aerospace medicine. Attendees practiced scanning for deep vein thrombosis, ocular and pulmonary findings, and renal/bladder assessment, each directly relevant to spaceflight physiology.
Many participants, whose only prior exposure to ultrasound was in obstetrics, gained a concrete appreciation for how POCUS functions, even in confined, resource-limited environments. The session concluded with open discussions on how these techniques might integrate into astronaut medical curricula and future lunar or Martian mission profiles.
Conclusion
Spaceflight point-of-care ultrasound (SPOCUS) represents both a technological innovation and an operational necessity. Yet, successful implementation hinges on training, engineering reliable equipment, image quality assurance, decision-support infrastructure, and rigorous validation of protocols in microgravity or simulated environments. It also depends on training skilled operators capable of independent, confident use far from Earth. Our OSMED workshop in Maui represents a timely and innovative step toward building a community of practitioners prepared for the unique challenges of “SPOCUS.” As space missions broaden to a lunar base and Mars, and as crew diversity expands, such training and research efforts are foundational for crew health, mission safety, and operational success.
Interested in OSMED? Reach out or join: https://www.osmed.org/
References
- Fischetti C, Frisch E, Loesche M, et al. Space Ultrasound: A Proposal for Competency-based Ultrasound Training for In-flight Space Medicine. West J Emerg Med. 2024;25(2):275-81.
- Asachi P, Ghanem G, Burton J, Aintablian H, Chiem A. Utility of ultrasound in managing acute medical conditions in space: a scoping review. Ultrasound J. 2023;15(1):47.
- Fischetti C, Rajagopal AB, Frisch EH, et al. SPOCUS©: Spaceflight Point-of-Care Ultrasound Training Curricula for Crew Medical Officers. SAGE Publications Sage CA: Los Angeles, CA; 2025. p. 10806032251330504.
- Anderson A, Theophanous RG. Point-of-care ultrasound use in austere environments: A scoping review. PLoS One. 2024;19(12):e0312017.
- Fox S, Fleshner M, Flanagan C, et al. Developing and evaluating a remote quality assurance system for point-of-care ultrasound for an internal medicine residency global health track. POCUS J. 2020;5(2):46-54.
- Lam J, Wong S, Grubic N, et al. Accelerated remote consultation tele-POCUS in cardiopulmonary assessment (ARCTICA). POCUS J. 2020;5(2):55-8.
- Ng KW, Gao Y, Furqan MS, et al. HoloPOCUS: Portable Mixed-Reality 3D Ultrasound Tracking, Reconstruction and Overlay. Springer; 2023:111-120.
 Hands-On learning during our SPOCUS course at the Inaugural OSMED Summit in Maui, HI in December 2024.
Hands-On learning during our SPOCUS course at the Inaugural OSMED Summit in Maui, HI in December 2024.
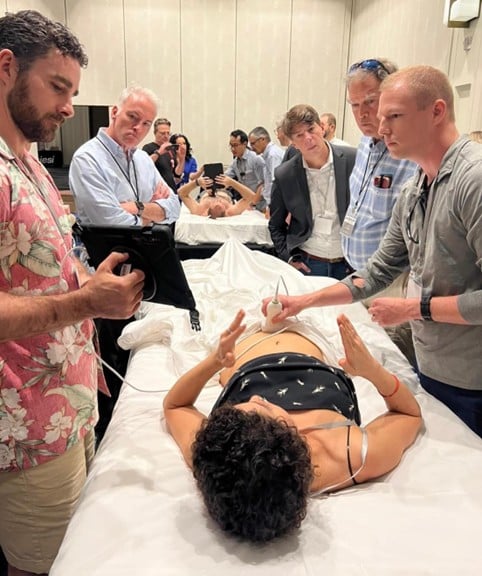 Learning how to bladder scan for in-flight urinary retention assessment
Learning how to bladder scan for in-flight urinary retention assessment
.