
Urine Trouble: Tricky Bladder Mimics
Kendra Jackson, MD, Pediatric Emergency Medicine Fellow, Atrium Health-Carolinas Medical Center, Levine Children’s Hospital
Peter Brooks, DO, Emergency Medicine Ultrasound Division, Atrium Health-Carolinas Medical Center, Levine Children’s Hospital
Lindsey Chaudoin, MD, Pediatric Emergency Medicine Ultrasound Director, Atrium Health-Carolinas Medical Center, Levine Children’s Hospital
Pediatric Case
A 13-year-old previously healthy female with no past medical history presented with 4 days of right lower quadrant pain. She had complete resolution of her pain after Motrin and a benign abdominal exam, so she was discharged home. She returned 4 days later with right lower quadrant pain, nausea, and vomiting that had reoccurred at 4 am that morning. A point-of-care ultrasound (POCUS) was performed and showed a normal bladder and no hydronephrosis. She had a normal transabdominal pelvic ultrasound for torsion and a non-diagnostic appendix ultrasound performed by radiology (Figure 1).
Her pain improved, and she was discharged home. She returned 24 hours later with 9/10 abdominal pain. On arrival, the patient received 4mg of morphine, 4mg of Zofran, and 1L of normal saline. Due to her persistent severe pain, she had an abdominal CT that was notable for a 10cm cystic lesion adjacent to the bladder and uterus (Figure 2). The radiologist noted the bladder was decompressed by the cyst. She was taken to the OR with gynecology and found to have a very large, edematous, and hemorrhagic right fallopian tube with hydrosalpinx. She was found to have a normal left fallopian tube and well-perfused bilateral ovaries. Her right fallopian tube was removed.
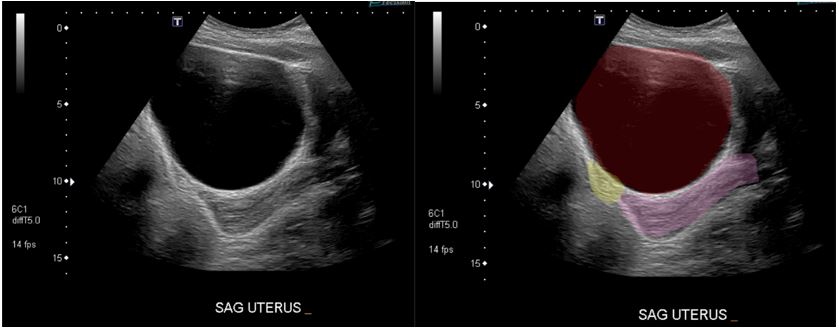
Figure 1: Transabdominal Ultrasound. Red: Hemorrhagic Hydrosalpinx; Pink: Uterus; Yellow: Bladder
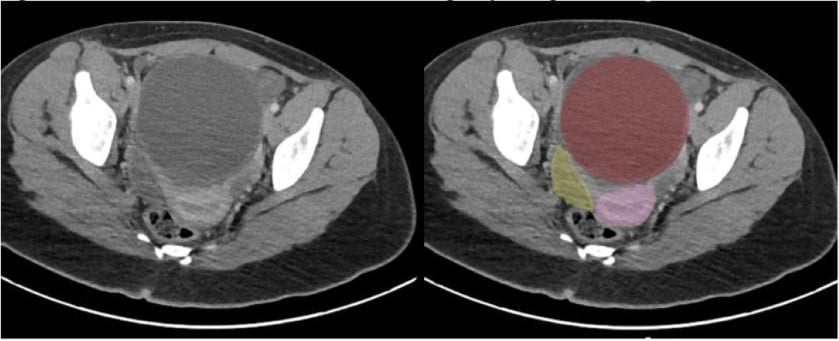
Figure 2: CT Abdomen and Pelvis. Red: Hemorrhagic Hydrosalpinx; Pink: Uterus; Yellow: Bladder
Adult Case
A 78-year-old female with a past medical history of recent CAD with NSTEMI and rectus sheath hematoma presented with severe abdominal pain via EMS. In transport, the highest heart rate was 35, and the lowest blood pressure was 93mmHg systolic. The patient had been discharged from rehabilitation four days prior to presentation. She reported mild pain at discharge that acutely worsened on the day of presentation. While the patient was being volume resuscitated, a RUSH exam was performed that showed severely reduced LVEF and a distended bladder. A foley was placed and minimal urine came out. The patient’s blood pressure and heart rate improved, and she was transported to the CT scanner, where a large pelvic hematoma was identified. The patient was taken for ex-lap and admitted to the surgical ICU.
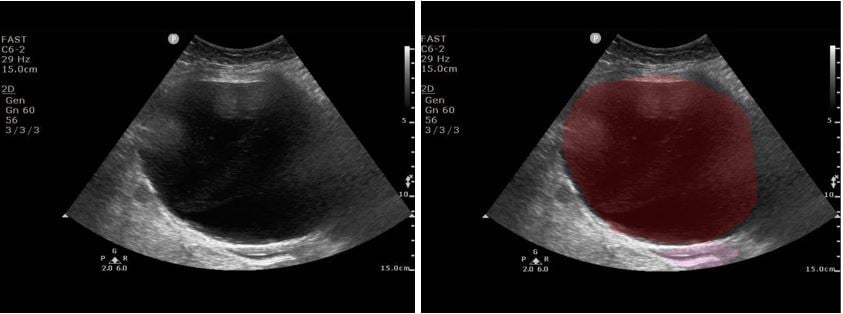
Figure 3. Bladder Ultrasound. Red: Hematoma; Pink: Uterus
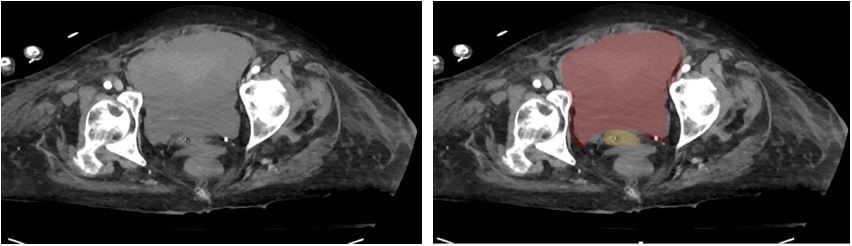
Figure 4. CT Abdomen and Pelvis. Red: Hematoma; Yellow: Bladder
Introduction
Bladder scans are essential to diagnosis, management, and treatment of emergency medicine patients. FAST and RUSH exams1 have incorporated bladder ultrasound to rapidly assess for free fluid in a hemodynamically unstable patient. For infants presenting with fever, POCUS can be used to assess bladder volume to facilitate timing of catheterization. For patients presenting with low urine output, POCUS can help differentiate low urine volume versus obstructive uropathy. Knowing the relevant landmarks, typical bladder shape, and mimics can help accurately identify pathology.
Technique
A thorough history is important to help providers interpret their POCUS images. Before performing the POCUS, ask the patient the timing of their last void and/or if they have the urge to best predict what you expect to see on ultrasound. Remember “LIMES”:
Landmarks
Start with your probe in sagittal, identify the pubic symphysis caudal to the bladder, the uterus or prostate posteriorly, and bowel gas cranially. In transverse, make sure you have enough depth to identify the rectum and uterus/prostate.
Without proper landmark identification, it is possible to mistake a collection of free fluid, an ovarian cyst, or a loop of distended small bowel for the bladder.
Interrogate
When fanning through the bladder, be sure to scan the entire bladder from left and right in sagittal, then superior to inferior in transverse to confirm your organ structure and any pathology.
Measure
In the sagittal view, measure the height of the bladder. In the transverse view, measure the depth and width of the bladder for an accurate assessment of bladder volume (Figure 5). If the volume is more than you expect, have the patient void, and rescan. If there is no change, consider adjacent anatomy that could mimic a bladder such as free fluid, pelvic hematoma, or an ovarian or fallopian tube pathology as in our cases. Though many providers “eyeball” volume, most ultrasounds have a measurement calculator to automatically calculate the volume for you, or you can calculate using the equation below.
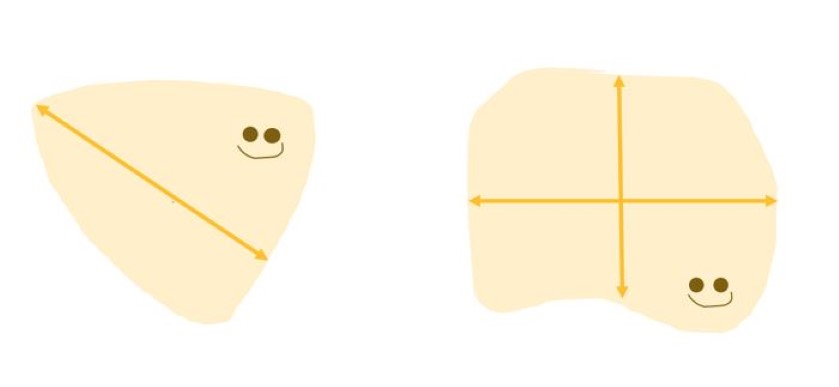
Figure 5: Bladder Volume Measurement2
Volume(mL) =Width(cm) x Depth(cm) x Height(cm) x 0.7
Bladder Volume By Age Equation3
<1 year: capacity (mL) = (2.5 x age [months]) + 38
>1 year: capacity (mL) = (2 + age [years]) x 30
Echogenicity
On ultrasound, urine should be anechoic. If the fluid is more complex, consider pelvic hematoma, ovarian/fallopian tube pathology or bladder debris such as in the setting of UTI or trauma.
Shape
Analyze the entire shape of the bladder by identifying the posterior and lateral walls. The bladder in sagittal is often shaped like a triangle, or a Dorito. In the transverse view, the most common bladder shape is cuboid, like a slice of pound cake. If the shape is not what you expect, have the patient void, and rescan.
Pre- & Post-Void
It is important when doing a bladder ultrasound to know when the patient last voided. A pre- and post-void ultrasound can help differentiate obstructive uropathy versus dehydration. Dilation of the renal pelvis can be secondary to urinary retention.
Discussion
Bladder point-of-care ultrasound is a high-yield study that can provide examiners with key information about volume status and obstructive uropathy. Bladder ultrasound has also been shown to decrease ED length of stay and expedite evaluation for ovarian pathology.4 Children who undergo CT scans have a significantly higher lifetime risk of cancer compared to those who do not,5 and this risk increases as the age at time of CT scan decreases. It is therefore important to minimize these CT scans when possible, in part by improving our sensitivity for intra-abdominal pathology with POCUS.
There are several pathologies that can be mistaken for the bladder.6,7 It is important to have a stepwise approach to POCUS of the bladder to ensure these pathologies are not missed. Knowing when the patient last voided can help examiners accurately interpret the obtained images. In our pediatric case, both the POCUS examiner and radiologist were fooled by the midline location and anechoic appearance of the hydrosalpinx. Having the patient void and rescanning would have shown no change in the structure and helped identify the pathology sooner. For our adult case, a foley was placed suspecting acute urinary retention, and not enough urine returned to account for the structure seen initially. This caused providers to be concerned that what they had identified as the bladder was not in fact the bladder, which CT confirmed. Landmarks are essential to orient the provider, to ensure that the image has the proper depth and to accurately identify pathology. Interrogating the entire bladder can help ensure that a small amount of free fluid in the pelvis is not missed. Measure the bladder volume and assess whether it is the appropriate size for age. Ensure the Echogenicity is what you expect. Complex fluid should be a cause for concern and reassessment. And finally, if the Shape is not what you expect, scan again after voiding. It’s easy to assume a large anechoic structure in the pelvis is the bladder. As more pediatric- and adult-trained emergency medicine providers become facile with POCUS, it is important that we go back to the basics to ensure thorough and complete exams.
References
- Seif D, Perera P, Mailhot T, Riley D, Mandavia D. Bedside ultrasound in resuscitation and the rapid ultrasound in shock protocol. Crit Care Res Pract. 2012;2012:503254.
- Bih LI, Ho CC, Tsai SJ, Lai YC, Chow W. Bladder shape impact on the accuracy of ultrasonic estimation of bladder volume. Arch Phys Med Rehabil. 1998;79(12).
- Guerra LA, Keays MA, Purser MJ, Wang SY, Leonard MP. Pediatric cystogram: Are we considering age-adjusted bladder capacity? Can Urol Assoc J. 2018;12(12):378-81.
- O’Brian RA, Firan A, Sheridan MJ, Kou M, Place RC, Chung CH. Bladder point-of-care ultrasound: A time saver in the pediatric emergency department. J Emerg Med. 2021;61(3):e32-e39.
- Mathews JD, Forsythe A v., Brady Z, et al. Cancer risk in 680 000 people exposed to computed tomography scans in childhood or adolescence: data linkage study of 11 million Australians. BMJ. 2013;346(May21):f2360-f2360.
- Smith TA. Not So FAST Part 3 - Bladder and Pelvis. Emory School of Medicine Case of the Month. Published September 2019. Accessed May 31, 2022.
- Estell D, Asanad K, Baker Z, Vasquez E. Mature ovarian cystic teratoma mimicking a bladder diverticulum in a 16-year-old female. Urology. 2021;149.



