
Cases That Count: Whirlpool Sign in Testicular Torsion
Romeo Wahome, MD, Emergency Medicine, Mbarara University of Science and Technology
Daniel Mirsch, DO, Clinical Assistant Professor Emergency Medicine, University at Buffalo
Matthew Churitch, MD, PGY-1 Emergency Medicine, University at Buffalo
Marisa Vallone-Bradfield, PA-C, Ultrasound Faculty Emergency Medicine, University at Buffalo
Case Presentation
A previously well, 14-year-old boy developed abdominal pain radiating to the right hemiscrotum two weeks prior to his evaluation in the emergency department (ED). He reported to have been playing in a football tournament on the day of the start of symptoms and subsequently went to a local clinic where he was diagnosed with orchitis. The patient was given antibiotics and analgesia, and instructed to return to the clinic a week later. However, he returned after four days due to increased pain in the left hemiscrotum. The clinic sent the patient to the ED after this second visit, where he presented with contralateral hemiscrotum pain. There were no other chronic medical conditions documented in this patient’s history, and he takes no medications except for the aforementioned prescriptions from the clinic. He reported normal food intake and bowel habits, and denied significant weight loss or night sweats.
On examination, vitals were normal, and the patient appeared overall nontoxic. The testicular examination revealed a markedly tender left testicle which was firm, nodular, and his pain was not relieved with raising of the testes. There were no masses, signs of hernias, superficial skin changes, or urethral discharge. The right testis was also firm, but noticeably less swollen.
Bedside ultrasound was performed, and in the transverse view of the left testis, the subcutaneous tissues look thickened. There was obvious edema noted, and mixed echogenicity within the testis indicated possible necrosis. There were no signs of gas or cobblestoning; however, the epididymis appeared thickened.
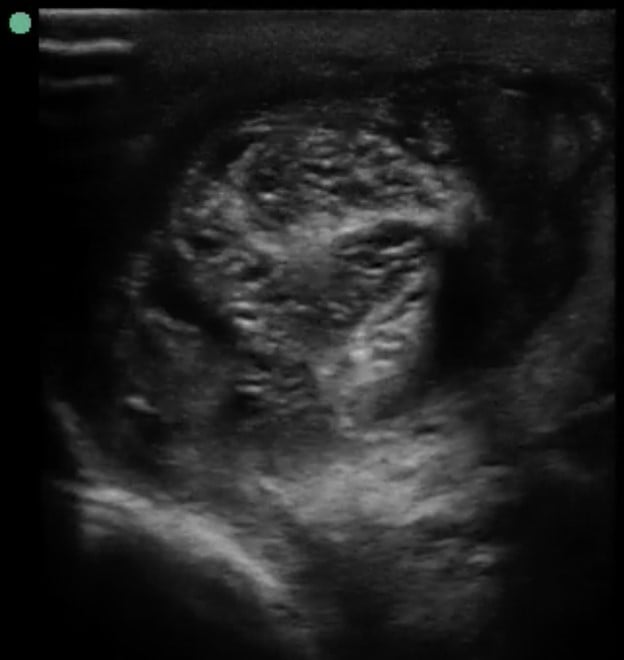
Image 1. Left proximal transverse view shows the whirlpool sign in the left spermatic cord.
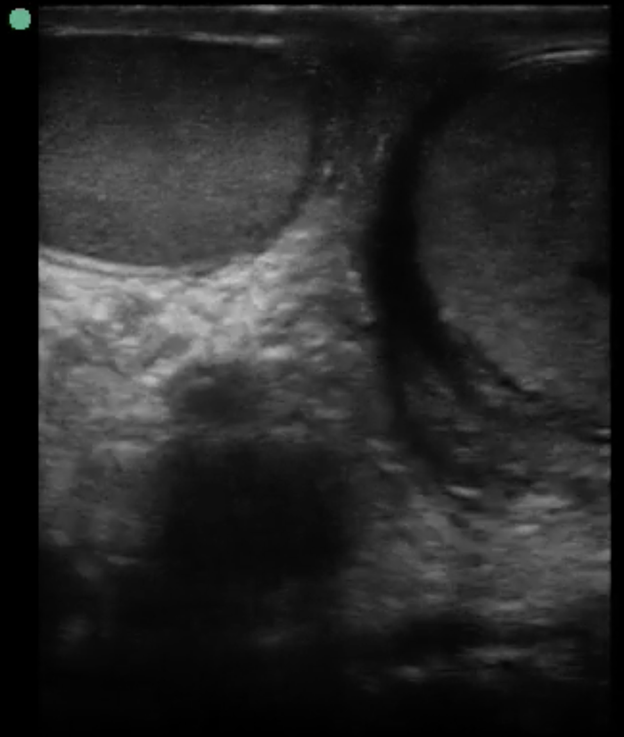
Image 2. Transverse “Buddy View” shows left predominant increased size of testis, heterogeneous echotexture, skin thickening, and mild hydrocele.
What is the whirlpool sign and why is it important?
The whirlpool sign seen on ultrasound can indicate twisting of the spermatic cord, suggesting persistent testicular torsion, in both partial and complete cases. With acute testicular torsions, it can take several hours before ischemic damage is evident on ultrasound.1 Early diagnosis is imperative for this condition, as every hour spent without treatment increases the likelihood of permanent damage to the affected testicle. Oftentimes, the presence or absence of Doppler flow can lead clinicians down the torsion pathway. Literature has shown that even when Doppler flow is present in the affected testicle, the presence of the whirlpool sign strongly suggests torsion.2 In 2007, Nicolas Kalfa et al performed a multi-center prospective trial that showed the whirlpool sign has a sensitivity and specificity of 81% and 100%, respectively, when read by a junior radiologist.3 Additionally, a 2018 meta-analysis by McDowall et al showed “a pooled sensitivity and specificity of the [whirlpool sign] of 0.73 (95% CI, 0.65-0.79) and 0.99 (95% CI, 0.92-0.99), respectively.”4 Thus, the sign is helpful in ruling in torsion, but not ruling it out.
Testicular Torsion Diagnosis
Testicular torsion is typically a combination of clinical diagnosis coupled with ultrasound findings.
Clinical Diagnosis
The clinical diagnosis can be organized by the TWIST score (Table 1), which was created in 2013 by JA Barbosa and has been prospectively validated in 2016, and most recently in January 2021.5-6 It is composed of 5 elements with varying point values with 0-2 being low-risk (torsion “excluded”), 3-4 moderate (ultrasound needed), and 5-7 high-risk (can go directly to the OR). A March 2022 meta-analysis by Qin et al showed a 98% sensitivity in low risk patients and a 97% specificity in high risk patients.7 Since this score is yet to be included in urology or emergency medicine guidelines, ED providers should still obtain a scrotal ultrasound on patients with an acute scrotal complaint. Ultrasound findings associated with testicular torsion are included in Table 2.
| TWIST Score Finding | Points |
| Testicular Swelling | 2 |
| Hard Testicle | 2 |
| Absent Cremasteric Reflex | 1 |
| Nausea Vomiting | 1 |
| High Riding Testis | 1 |
Table 1. TWIST Score
Ultrasound Diagnosis
There are several signs of testicular torsion on scrotal ultrasound. Starting from the superior aspect, the spermatic cord can be seen with a whirlpool sign (knot-like) when compared to the unaffected side. This sign has high specificity with low sensitivity in Baud et al.,8 from 1998 and again demonstrated in McDowall’s meta-analysis in 2018.4 For now, the sign rules in testicular torsion but does not rule it out. Several other signs will favor the diagnosis, such as: spiral-like flow on color Doppler, an up-tracking epididymis as it is being dragged towards the inguinal canal, or an increased testicular size compared to a normal contralateral testis.
Arterial waveform resistive index (RI) is one of the most sensitive and specific tests for testicular torsion. The RI is calculated when an arterial waveform is identified (arterial has prominent pulsations compared to the more flat and unchanging venous waveform), and a pulse wave Doppler tracing shows peak systolic velocity and lowest diastolic velocity. The formula for calculating this is noted in Figure 1 and an example waveform in Figure 2. A normal RI is 0.5-0.7. Echogenicity of the testicle also changes over time as parenchymal bleeding builds, causing increased brightness on the affected side. As this bleeding occurs sporadically, the echotexture becomes increasingly varied, causing heterogeneous echogenicity.
A hydrocele is common in acute torsion, as inflammatory edema builds in the surrounding tissue. However, it can be absent in chronic torsion. Scrotal skin edema and thickening may also be present.
| Ultrasound Findings in Acute Testicular Torsion9 |
| Whirlpool sign on grayscale |
| Whirlpool sign on power Doppler |
| Arterial waveform resistive index > 0.75 or absent |
| Increased size of testis or epididymis |
| Heterogeneous echotexture |
| Hydrocele |
| Scrotal skin thickening or hyperemia |
Table 2. Ultrasound findings in acute testicular torsion
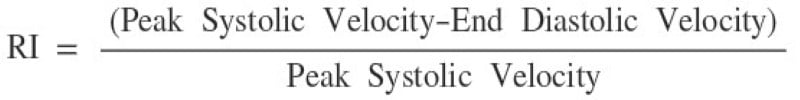
Figure 1. Resistive index formula for arterial waveforms
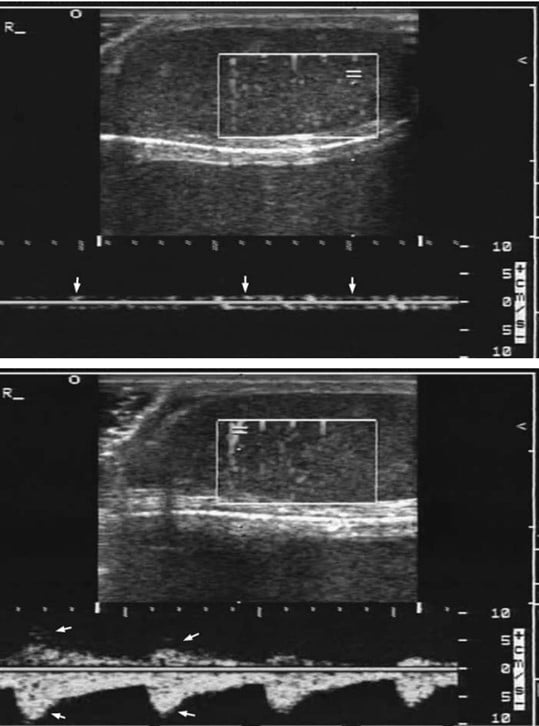
Figure 2. Examples of a normal testicular venous waveform (upper panel) and an arterial waveform (lower panel)10
Technique
The high-frequency probe (at least 7.5 MHz) should be used to evaluate the testicle. Ideally, the patient should be supine, knees bent with the hips externally rotated (frog leg position). The unaffected side should be scanned first in order to establish a baseline. Fully scan each testis, epididymis, and spermatic cord in both the longitudinal and transverse planes, starting medially and moving laterally. The portion of spermatic cord superior to the epididymis is where the whirlpool sign can be seen. It is imperative to obtain the view that includes both testes in order to evaluate for asymmetry, which is known as the “Buddy View.” Finally, color or power Doppler (the latter is more sensitive in low flow states but cannot differentiate direction) can evaluate for the presence or absence of blood flow to each testicle.11 The Doppler mode of choice should be power Doppler (which is up to 5 times more sensitive than color Doppler) to detect the “slow-moving” blood in the testes [10]. In case of ongoing torsion, the affected testicle will appear hypoechoic compared to the unaffected side as a result of edema and eventual necrosis.10
Case Resolution
The patient went to the operating room where the left testicle was found to be necrotic and was subsequently removed. The right testicle had an orchiopexy performed.
Summary
Ultrasound is the best imaging modality for the acute scrotum. The whirlpool sign is one of the most specific findings available and should be considered highly indicative of acute testicular torsion in the appropriate clinical context. An emergent urologic consult should be placed when acute testicular torsion is suspected.
References
- Vijayaraghavan SB. Sonographic differential diagnosis of acute scrotum: real-time whirlpool sign, a key sign of torsion. J Ultrasound Med. 2006;25(5):563-74.
- Nishizawa T, Kobayashi D, Uematsu H, et al. Ultrasonographic ‘whirlpool sign’ in testicular torsion. BMJ Case Report. 2021;14:e241638.
- Kalfa N, Veyrac C, Lopez M, et al. Multicenter assessment of ultrasound of the spermatic cord in children with acute scrotum. J Urol. 2007; 177(1):297-301; discussion 301.
- McDowall J, Adam A, Gerber L, et al. The ultrasonographic "whirlpool sign" in testicular torsion: valuable tool or waste of valuable time? A systematic review and meta-analysis. Emerg Radiol. 2018;25(3):281-292.
- Barbosa JA, Tiseo BC, Barayan GA, et al. Development and initial validation of a scoring system to diagnose testicular torsion in children [published correction appears in J Urol. 2014 Aug;192(2):619]. J Urol. 2013;189(5):1859-1864.
- Sheth KR, Keays M, Grimsby GM, et al. Diagnosing Testicular Torsion before Urological Consultation and Imaging: Validation of the TWIST Score. J Urol. 2016;195(6):1870-1876.
- Qin KR, Qu LG. Diagnosing with a TWIST: Systematic Review and Meta-Analysis of a Testicular Torsion Risk Score. J Urol. 2022;208(1):62-70.
- Baud C, Veyrac C, Couture A, Ferran JL. Spiral twist of the spermatic cord: a reliable sign of testicular torsion. Pediatr Radiol. 1998;28(12):950-954.
- Gaillard F, Jones J. Testicular torsion. Radiopaedia.org. October 4, 2010. Accessed November 1, 2021. https://radiopaedia.org/articles/10959
- Blaivas M, Brannam L. Testicular ultrasound. Emerg Med Clin North Am. 2004; 22(3):723-48, ix.
- Adhikari S. “Testicular.” In: Ma O, Mateer JR, Reardon RF, Byars DV, Knapp BJ, Laudenbach AP. eds. Ma and Mateer's Emergency Ultrasound, 4e. McGraw Hill; 2021.
Additional Resources
- Hasan O, Mubarak M, Mohamed Jawad Alwedaie S, et al. Ultrasound heterogeneity as an indicator of testicular salvage in testicular torsion: A single center experience. Asian J Urol. 2022;9(1):57-62.
- Prando D. Torsion of the spermatic cord: the main grayscale and doppler sonographic signs. Abdom Imaging. 2009;34(5):648-661.
- Schmitz D, Safranek S. Clinical inquiries. How useful is a physical exam in diagnosing testicular torsion? J Fam Pract. 2009;58(8):433-4.
- Shih, J. Ultrasound for the win: 22M with scrotal pain #US4TW. ALiEM. July 19, 2017. Accessed April 15, 2022.
- Zheng WX, Hou GD, Zhang W et al. Establishment and internal validation of preoperative nomograms for predicting the possibility of testicular salvage in patients with testicular torsion. Asian J Androl. 2021;23(1):97-102.



