Immersive Technologies in Emergency Medicine Education: Integrating Virtual and Augmented Reality into Ultrasound and Simulation Training
Nelson Escuerdo-Gorritz, MD
Colton Southall, MD, MBA
Solomon Sebt, MD
This article is a collaborative effort between the ACEP Emergency Ultrasound Section Simulation and Fellow Education Subcommittees. Thank you to everyone.
Introduction
In the world of graduate medical education (GME), a silent revolution is underway, and in the spirit of advancing medicine, it has become digital. This meaningful and transformative change encompasses the new frontiers of virtual reality (VR), augmented reality (AR), and mixed reality (MR) - collectively referred to as extended reality (XR). These technologies are increasingly being integrated into medical education. What was once thought of as science fiction from yesteryear is now an actuality. In emergency medicine (EM), where procedural dexterity, rapid decision-making skills, and team coordination are quintessential tenets of the craft and practice, XR offers unique frontiers that supplement traditional teaching modalities in simulation and bedside instruction. This newsletter explores how these tools can be thoughtfully incorporated in ultrasound (US) and simulation-based didactics, grounded in education theory and current evidence-based practices.
Educational Theories Behind XR Integration
Current XR-based education effectiveness lies within several complementary learning theories:
- Experiential Learning
David A. Kolb’s 1984 theory on learning helps espouse current VR and AR immersion to facilitate environments for learners to actively experience, reflect, conceptualize, and experiment - his four-stage learning cycle.1 It is relevant to EM, where reflection and repetition in complex scenarios are crucial to real-life clinical scenarios, albeit limited. - Cognitive Load
XR environments have the potential to reduce extraneous cognitive load by guiding learners through complex psychomotor tasks with visual cues, commonly referred to as overlays. This controls what the learner is presented and therefore controls their focus and lessens cognitive resources and overload. This facilitates conceptual understanding of underlying principles. 2 - Deliberate Learning and Mastery
Simulation and ultrasound in EM training benefit the learner with repetition, immediate feedback, and progress after achieving competence. XR tools allow for scalable, individualized, and low-risk deliberate practice outside of scheduled labs. - Situated Learning
XR posits the learner in realistic and contextually enriched scenarios. Examples include replication of resuscitation bays or trauma suites - allowing for the transfer of knowledge, situational awareness, and critical elements of emergency care.
Application Examples for Emergency Medicine Training
- Ultrasound Education - enhancing spatial reasoning and psychomotor skills
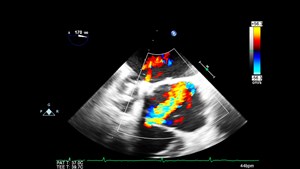
Point-of-Care Ultrasound (POCUS), now nearing ubiquity in emergency departments, requires integrating visuospatial reasoning, fine psychomotor control, and anatomical knowledge. A common challenge of novice ultrasound learners is how to translate a two-dimensional image into a three-dimensional mental map.
VR ultrasound simulators create immersive and interactive experiences that aim to help bridge this gap. SonoSim® VR and CAE Vimedix®, pioneers in this vision, replicate probe handling, tissue feedback, and pathologic image variation. Studies show that VR-based POCUS training improves image interpretation and probe orientation compared to traditional didactics alone. 3,4
AR overlays extend this aforementioned capability by projecting holographic anatomical structures, such as ideal probe positions, onto the task trainer or live model. This allows the learner to visualize target anatomy, needle trajectory, and sonoanatomy in real-time, improving procedural accuracy and retention.5,6 AR guided learning reinforces this visuomotor integration via continuous visual feedback - an educational advantage that even skilled instructors can not perfectly replicate.
- Team-Based Training
The specialty of emergency medicine thrives on interprofessional teamwork and crisis resource management. Traditional in-situ simulation, while effective, can be logistically limited - requiring space, manikins, trained staff, and scheduling coordination. Circumventing this, multi-user VR platforms enable team distribution to engage in shared, immersive resuscitation scenarios. Participants interact within a virtual ED, perform assessments, communicate via voice recognition, and can manage critically ill patients under a time clock. It allows for anxiety reduction across all populations, especially in pediatric and adolescent populations, with one person in front of them as opposed to many, fostering a better environment for better patient care and outcomes.7
Multiple studies have demonstrated that VR-based team training enhances CRM performance, communication, and leadership behaviors comparable to conventional high-fidelity simulation.8 Moreover, VR provides automated data capture to facilitate objective debriefing and competency assessments. Extending into real-world encounters and high-patient populations, it reduces harmful exposure but retains maximum learning through virtual reality in real time.10
- Procedural Skill Acquisition
VR procedural modules replicate high-stakes interventions such as airway management, thoracostomy, thoracotomy, and ultrasound-guided vascular access. Participants can repeat procedures in a psychologically safe environment to receive immediate and standardized feedback on performance metrics (eg, needle angle, insertion depth, time to completion).
AR-assisted procedures - using headsets like Microsoft’s HoloLens or other AR-enhanced tablets - display real-time visual guides aligned with the learner’s field of view. In pilot studies, AR guidance improved accuracy in central venous catheterization and reduced needle redirections compared to traditional instruction.9,10 This type of “visual coaching” allows junior residents and medical students to internalize proper ergonomics and procedural flow before performing on real patients.
Formal Implementation into Residency Programs
Step 1: Curricular Alignment
Identify specific learning objectives that XR can uniquely enhance for the needs of the program - should be objective-driven, not technologically driven.
Step 2: Blended Learning Design
Combining VR and AR sessions with live supervision and bedside application.
Evidence supports blended approaches as opposed to standalone digital learning.10 The use of VR allows for foundational exposure, and AR reinforces tactile and contextual learning.
Step 3: Assessment and Feedback
Utilize built-in performance metrics for formative feedback. Examples include - time to completion, accuracy, and error rate. Incorporating these data into milestones or entrustable professional activity (EPA) evaluation fosters objective competency tracking.
Step 4: Faculty Development
Train small groups to become “XR champions” among ultrasound and simulation faculty, in this case, dedicated simulation and ultrasound fellows. Those trained should have comfort and enthusiasm, which strongly predict successful adoption.
Step 5: Scalability and Access
Pilot modules, such as cardiac ultrasound (VR measure) or venous/arterial line placement (AR measure), allow for easier facilitation as these are common procedures within an ED. Rotating in small group sessions during dedicated didactic days ensures equitable access and maintenance of skills.
Educational and Operational Benefits of XR Integration
Going beyond formal skill acquisition, XR training allows for 1) standardization - ensures every learner encounters the same pathology and procedural steps; 2) equity - democratizes access to high - quality training, independent of institutional simulation resources; 3) efficiency - reduces reliance on limited physical resources and limited time; 4) safety - allows for risk-free repetition of high acuity, low occurrence (HALO) or other hazardous procedures; 5) evidence based education - enables objective performed analytics and tailored, individualized remediation and progression.
The Future of XR Simulation-Based Educational Media and Conclusion
Despite strong promises backed by data, several barriers remain:
- Cost of infrastructure - program/GME budgets, headsets, software licenses, integration with existing electronic health records, and routine maintenance of devices.
- Faculty preparedness - technical and pedagogical training required, the need for a trained simulation or ultrasound-trained fellow/attending.
- Motion sickness and accessibility - can limit session duration and therefore education. The need for an alternative is essential for those who are prone.
- Modification of reality - XR can cause the loss of realism, much like motion sickness, for a specific procedure or organ structure, and therefore impede learning.11
- Research heterogeneity - current research has a wide variation in study design and outcome measurements, limiting testable outcomes to real-life patient outcomes.
Future research should shift its focus to longitudinal outcomes. XR-based training impacts patient care, procedural success, and error reduction. One meta-analysis focused on cardiopulmonary resuscitation training, a critical procedure within an ED, and revealed that of the nine random clinically controlled trials, that the XR methods were just as effective as face - to - face instruction for procedural competency, but did not demonstrate statistical significance in superiority.12 There was no mention of long-term patient follow-up when comparing the XR-trained groups and the traditional face-to-face groups. Integration with learning management systems can potentiate further personalization and streamline competency tracking.
Virtual and augmented realities represent the next logistical evolution in simulation and ultrasound education within emergency medicine. It is the intersection of rapidly evolving technology and the next generation of healthcare workers. When grounded in sound education theory and data and implemented through blended equitable approaches, these tools can meaningfully enhance emergency procedural mastery, team performance, and clinical reasoning. As medical educators, the goal is not to replace bedside teaching but to enhance preparedness, efficiency, and safety.
References
- Mcleod S. Kolb’s Learning Styles and Experiential Learning Cycle. Simply Psychology. Published March 19, 2025. https://www.simplypsychology.org/learning-kolb.html
- Sweller J. Cognitive Load during Problem solving: Effects on Learning. Cognitive Science. 1988;12(2):257-285.
- Andersen NL, Jensen RO, Konge L, et al. Immersive Virtual Reality in Basic Point-of-Care Ultrasound Training: A Randomized Controlled Trial. Ultrasound Med Biol. 2023;49(1):178-85.
- Abbas JR, Chu MMH, Jeyarajah C, et al. Virtual reality in simulation-based emergency skills training: A systematic review with a narrative synthesis. Resusc Plus. 2023;16:100484.
- Liao SC, Shao SC, Gao SY, Lai EC. Augmented reality visualization for ultrasound-guided interventions: a pilot randomized crossover trial to assess trainee performance and cognitive load. BMC Med Educ. 2024;24(1):1058.
- Tang KS, Cheng DL, Mi E, Greenberg PB. Augmented reality in medical education: a systematic review. Can Med Educ J. 2020;11(1):e81-e96.
- Extended Reality Is Radically Changing the World of Medicine. Michiganmedicine.org. Published August 24, 2021. Accessed February 5, 2026. https://www.michiganmedicine.org/medicine-michigan/extended-reality-radically-changing-world-medicine
- Lerner D, Mohr S, Schild J, Göring M, Luiz T. An Immersive Multi-User Virtual Reality for Emergency Simulation Training: Usability Study. JMIR Serious Games. 2020;8(3):e18822.
- Boogaard LL, Notten K, Kluivers K, Van der Wal S, Maal TJJ, Verhamme L. Accuracy of augmented reality-guided needle placement for pulsed radiofrequency treatment of pudendal neuralgia: a pilot study on a phantom model. PeerJ. 2024;12:e17127.
- Tene T, Vique López DF, Valverde Aguirre PE, Orna Puente LM, Vacacela Gomez C. Virtual reality and augmented reality in medical education: an umbrella review. Front Digit Health. 2024;6:1365345.
- Castillo-Rodríguez JM, Gómez-Urquiza JL, García-Oliva S, Suleiman-Martos N. Effectiveness of Virtual and Augmented Reality for Emergency Healthcare Training: A Randomized Controlled Trial. Healthcare (Basel). 2025;13(9):1034.
- Sun R, Wang Y, Wu Q, et al. Effectiveness of virtual and augmented reality for cardiopulmonary resuscitation training: a systematic review and meta-analysis. BMC Med Educ. 2024;24(1):730.
Educational Simulation Case Example
The learner enters the simulation room and should be able to place a virtual headset and handheld devices; the headset is connected to audio for the examiner for feedback.
Examiner Introductory Statements
Examiner: “Hello, Dr. (Candidate name). I am Dr. (Examiner name), welcome to your simulation training. I will be your examiner for this 15-minute simulation case. As a reminder, with the headset and equipment, I am happy to adjust any settings, such as volume, brightness, and the positioning of the patient. Reminder, this will mimic real-life scenarios and you should verbalize your thoughts, actions, and needs as appropriate and as able. Before we started, did you have any questions?”
Case Introduction
“The patient is a 21-year-old male college student playing in his senior ice hockey championship game as a goalie. While taking a quick water break, a rival team member took a wrist shot, and the puck made direct contact with his face. He is swiftly brought to the ED by his coach and team physician, complaining of left eye pain and swelling. On examination, you notice the patient is in significant distress, although overall hemodynamically stable, and you identify significant left peri-orbital swelling. During your initial evaluation, the patient can not open his left eye without assistance, and visual acuity is 10/100. Light is not painful. The patient has a fixed and dilated pupil with chemosis and limited extraocular motion, and IOP is 45 mmHg. His right eye is within normal limits, and visual acuity is 20/20. IOP is 10 mmHg and movement is intact.”
The patient is seen on the gurney, through a headset, and is actively in pain and complaining of decreased vision.
Learner/Patient History
Case assesses the learner’s ability to obtain relevant history
- No significant past medical or family history, medications, surgeries, or social history
- HPI: Struck by a hockey puck at high speed to the left peri-orbital region. No LOC. A+Ox4, GCS 15. A 15-point review of systems is overall negative except for pain in the affected region.
- If a full physical exam is requested by the learner, the examiner will provide for all asked organ systems, which will be negative for the affected peri-orbital region as described and will be repeated.
Task Completion
Examiner: “Now that you have the necessary information, what are your differential diagnoses, and what do you think is next in caring for this patient?”
Case will also assess the learner’s capacity to recognize and verbalize that the patient may have either orbital compartment syndrome or a retrobulbar hematoma, among other differentials.
- Expected to mobilize the patient to a resuscitation bay
- Expected to call for an emergent ophthalmology consult
Examiner: “The unit secretary reached out to them and said they are an hour away, and 'do what you need to do for the patient', and hung up.
- Should prompt nursing staff to obtain IV access, obtain lab work, and give IV analgesic of choice; consider procedural sedation
- Should prompt for Tdap vaccine status or pre-emptively give a Tdap vaccine
- Should order a STAT CT maxillofacial and orbits with contrast
Examiner: “Now that you have identified what procedure you want to do, what materials do you want?”
- Learner expected to call for either a suture repair kit with a 27g needle and 10cc anesthetic of choice, chlorhexadine/iodine
- Can call for hemostats, iris scissors, forceps, and drapes instead of a suture repair kit
- Materials will appear on the screen after being called out by the learner
Examiner: “ Now, please proceed with the procedure.”
- Learner must clean and drape the affected and planned site first and then inject local anesthesia into the lateral and inferior orbital rim, taking care to avoid the syringe bevel with the orbit.
- Next, take the forceps/hemostat and clamp the lateral canthus for 1 minute and then release
- Learner should then take the iris scissors and cut the area that was clamped down to the tendon and expose it
- Learner should pull the lower eyelid away to expose the lateral canthus and inferior lateral canthal tendon.
- Learner should be prompted upon visualization that it’s a white fibrous band
- Learner should then cut through the inferior tendon at the crus
- Learner should re-assess IOP (which will be normal)
Examiner: “If the patient still has increased IOP? What would the next step be?”
- Learner should verbalize they would cut the superior lateral canthal tendon. Should reassess the patient as vision can come back in 15 mins to 6 hours.
Closing Statement
Examiner: “Thank you, Dr. (Candidate Name), that concludes your case.”
- If the learner had difficulty, “I would like to draw attention to this video”: https://medvr.education/solution/lateral-canthotomy/
Education takeaway for learner: immediate action should be taken to recognize ocular emergency and perform an emergent procedure in the setting of a tonopen contraindication. Learners should provide steps or ask for help when performing the procedure, if necessary, for guidance. Learners should recognize time sensitivity and act in accordance with the current emergency medicine procedure guideline to perform a lateral canthotomy, an emergent procedure, when indicated.
References
- Ostrowski K, Miers J. Procedure: Lateral Canthotomy. Life in the Fast Lane • LITFL. Published April 8, 2025. https://litfl.com/procedure-lateral-canthotomy/
- Pham B, Lin B, Pham R. How to perform a lateral canthotomy. EyeGuru.org. Published January 25, 2020. https://eyeguru.org/blog/lateral-canthotomy/
- Gunderman M. Lateral Canthotomy and Cantholysis. University of Cincinnati Medical Center. 2014, updated 2018. Accessed February 5, 2026. https://www.uchealth.com/wp-content/uploads/sites/98/2018/02/Procedure_Lateral-Canthotomy-and-Cantholysis_CLIN64.pdf